Abstract
OBJECTIVE To investigate the significance of angiogenesis of lung cancer, in order to provide a scientific basis for interventional therapy.
METHODS Double-phase enhancement-scanning spiral CT and DSA were performed in 56 pathologically confirmed lung cancer cases, in order to evaluate angiogenesis of the tumors. The patients included 36 males and 20 females, with ages ranging from 33 to 76 years (average of 53). Assessments and indexes for SCT and DSA examinations were as follows: a) Peak value (PV) of the cancerous focus was the difference between the maximum CT value after enhancement and the CT value of a plain scan; b) The abnormally distorted and expanded new vessels of the cancerous focus which could be macroscopically discriminated; c) DSA staining of the focus of cancer was sparse, grid-like and dense. Chemotherapy and embolotherapy via the bronchial artery (interventional therapy) were conducted. Radiotherapy was added for some of the solid tumors with a diameter exceeding 4 cm.
RESULTS a) There were 25 cases with a central-type lesion, among which 4 were small cell lung cancers (SCLC) and 21 non-small cell lung cancers (NSCLC). The cases with a peripheral location accounted for 31 of the total, with a maximum diameter of 1.5 to 13.5 cm and a median of 4.2 cm, including 5 small cell lung cancers and 26 NSCLC cases. b) The reinforced PVs of the cancerous foci were as follows: The PV ranged from 45 to 70 Hu in 34 cases, 25 to 45 Hu in 19, and 10 to 25 Hu in 3. Sparse DSA staining occurred in 3 cases, there was uneven grid-like staining in 22 and dense staining in 31; c) The interventional therapy via the bronchial artery was conducted twice in 5 cases with the SCLC, and three times in 4 SCLC cases. For 3 of the latter cases, a dose of 5,000 to 7,000 cGy radiation therapy was added during the interventional treatment. Complete remissions (CR) were seen in 88.9% of the cases (8/9) and partial remission (PR) in 11.1% (1/9). Interventional therapy was conducted twice in 8 cases with NSCLC and three times in 30 with NSCLC and four times in 9 cases. Among the total cases, 13 received radiotherapy during interventional therapy, with a radiation dose of 5,000-7,000 cGy; The CR rate was 78.7% (37/47), PR was 14.9% (7/47) and the rate of non-remission was 6.4% (3/47).
CONCLUSION Using imaging technology, analysis of angiogenesis of lung cancers was employed to accurately detect and quantify angiogenesis. This analysis was combined for interventional therapy, using embolizing agents and large doses of the anti-tumor drugs and angiogenesis inhibitors. The agents were selectively delivered into the tumor vessels to eliminate the primary tumor, in order to depress distant metastases and thus enhance the curative effect of the therapy.
keywords
INTRODUCTION
Lung cancer is one of the most common human malignancies, with an increasingly incidence and morbidity. Angiogenesis of tumors plays an important role in all phases of tumorigenesis, development, infiltration and metastasis of solid tumors, and significantly influences the cancer biological behaviour and prognosis of the patients[1-3]. At present, there have been few clinical reports from China regarding interventional therapy in which accurate detection and quantification of angiogenesis of lung cancers were studied using imaging technology or other techniques. To provide information that will be of value for interventional and combined tumor therapy, we have analyzed angiogenesis of 56 cases of the lung cancer treated during the period from 2000 to 2005.
MATERIALS AND METHODS
Selection of the cases
A total of 56 cases with lung cancer were selected, with 36 male and 20 female patients. The age of the patients ranged from 33 to 76 years, with an average of 53.
Equipment and contrast materials
Double-phase CT enhancement scanning: The Pick Sele-SP type CT and US 310—P high-pressure syringe, made in the U.S was used. The thickness of the double-phase enhancement scanning was 2.0 to 5.0 mm, the interlaminar space was 3.0 to 5.0 mm, and the pitch was 1.0. A solution of 100 ml of Shuangbei iohexol was employed as a contrast material. A bolus injection of 2.0 ml/s was administered. Following the injection, 25 s arterial-phase and 50 s venous–phase scans were conducted. The Italian SIAS DVS2000 type arm C angioGyaphic apparatus and the U.S. LF-6000 type high-pressure syringe were employed, with the Seidingger technology. A lead-in ductus was used for the bronchial arteriography. For the arteriography a dose of 10 ml of Omnipaque was used as the contrast agent, administered at a velocity of 2.0~3.0 ml/s with a total volume of 9~15 ml. The 6 frame frequencies/s were applied for image collection at the arterial phase and 3 frame frequencies/s for the parenchymal phase.
The assessments and indexes of the SCT and DSA observation: ①The peak value (PV) of the cancerous focus was the difference between the maximum CT value after enhancement and the CT value of the plain scan. ②The image manipulation: Functional, a CT software, was utilized to edit and analyze the pattern of tumor blood-flow perfusion. ③The DSA staining of the cancerous focus: sparseness, reticulation and denseness.
RESULTS
There were 25 cases with central-type tumors, among which 4 were SCLC and 21 NSCLC. The patients with peripheral tumors accounted for 31 of the total, with a diameter range of 1.5 cm to 13.5 cm and a median of 4.2 cm. These included 5 SCLC and 26 NSCLC cases.
The reinforced PVs of the cancerous focus were as follows: The PV ranged from 45 to 70 Hu in 34 cases, 25 to 45 Hu in 19, and 10 to 25 Hu in 3; For the DSA staining, sparse staining occurred in 3 cases, uneven grid-like staining in 22 and dense staining in 31; In the pattern of blood-flow perfusion of the tumors with Functional software color coding, there were 15 cases with abnormal arteriolae, 9 with an anomalous bloodlake (sinus) video image and 32 with a stamen or pistil-shaped image.
The interventional therapy of the bronchial artery was conducted twice in 5 cases with SCLC, and it was performed three times in 4 SCLC cases. Among these cases, a dose of 5,000 to 7,000 cGy radiation therapy was added during the interventional treatment of 3 cases, with complete remission (CR) in 88.9% (8/9) and partial remission (PR) in 11.1% (1/9). Interventional therapy was conducted twice in 8 SCLC cases, three times in 30 NSCLC cases and four times in 9. Of the total cases, radiotherapy during the interventional therapy was added in 13, with a radiation dose of 5,000~7,000 cGy. The CR rate was 78.7% (37/47), the PR was 14.9% (7/47) and the rate of nonremission was 6.4% (3/47).
DISCUSSION
Over the past few years, continuous significant progress has been made in the application of molecular biology in cancer research. Oncogenic mechanisms of are gradually being understood at the molecular level. At the present time, there are a number of laboratories involved in basic studies and preclinical research on tumor angiogenesis, but clinical research has just begun. Now angiogenic studies on breast cancer rank first, followed by research on cancer of the uterine cervix, bone and nervous system[4]. However, there have been few reports from China on the assessment of angiogenesis in lung cancer, along with interventional therapy. Carmeliet et al.[5] have observed that tumor malignancy was related to new peripheral vessels. Distribution of the blood vessels in the small tumors was even, however, distribution of the blood vessels in various parts as the tumor growth became more asymmetric. There were many tumor frontline or peripheral vessels but fewer central vessels. Frequent bending of the vessels and enhancement of the blood viscosity occurred with angiogenesis of necrotic tumors, thus preventing the blood from transporting drugs into the tumors. These conditions also occurred in the sites with a rich blood supply. The disordered tumor structure and abnormal blood flow directly affected the curative effect of a venous administration route.
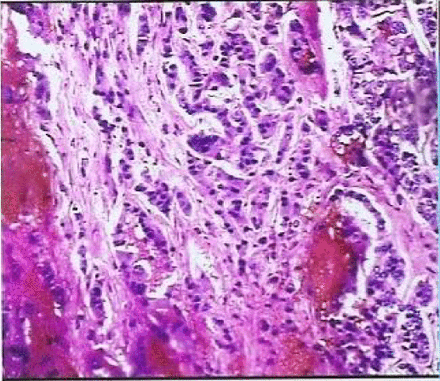
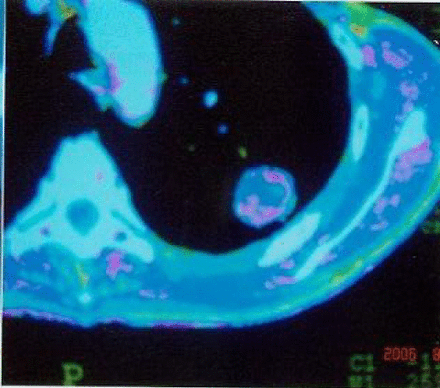
An important part of our study was to develop imaging technology in order to accurately locate and quantify tumor angiogenesis. Early technology for fast enhancement using spiral CT for tumor diagnosis was initiated for studies of angiogenesis and was the most fundamental qualitative assessment. The DSA staining of cancerous foci can be used to judge the extent of the malignancy. After the double-phase enhancement scanning employing spiral CT and DSA staining of the cancerous foci of the 56 lung cancer cases, we found three results as follows: ①The higher extent of malignancy, correlated with the larger numerical value of intensified value (PV) of the cancer foci; ②The blood-flow perfusion became clearer as the grid-like DSA staining became more dense; and ③The metastatic lymph nodes in the mediastinum and lung hilus were also intensified and stained as the display of abnormal arteriolae and new vessels became more limpid. There was less blood supply to the center of the major solid tumor caused by necrosis and liquification and there were new vessels with anomalous twists and expansion around the cancerous foci. Compared to that at the tumor borderline, the blood flow was significantly increased to the center of the tumor. There was no or little indication of blood flow in the necrotic area (Figs.1~4).
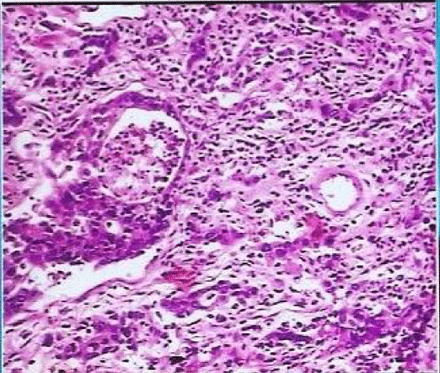
New vessels of poorly differentiated squamous cell carcinoma
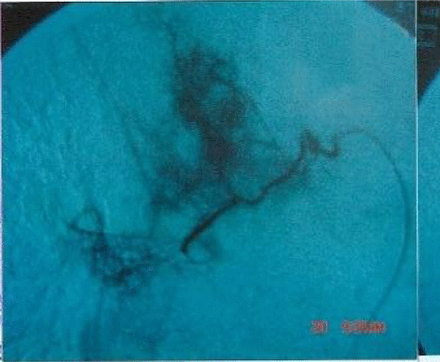
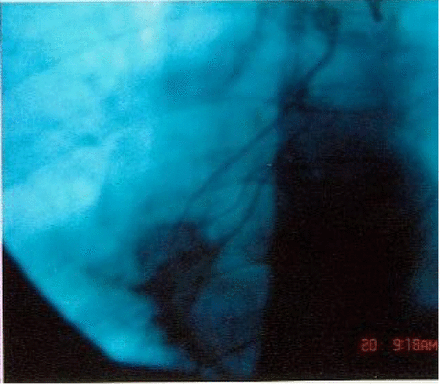
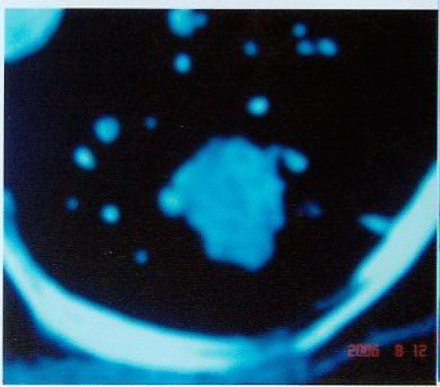
DSA image before treatment of the same case
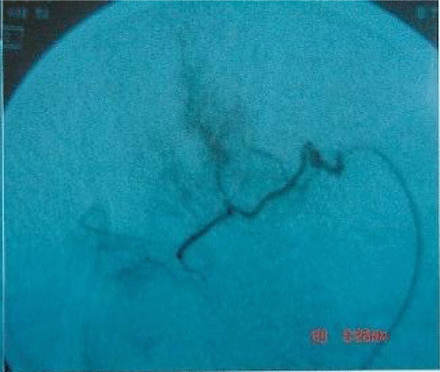
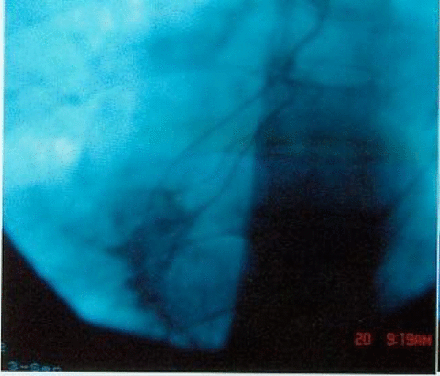
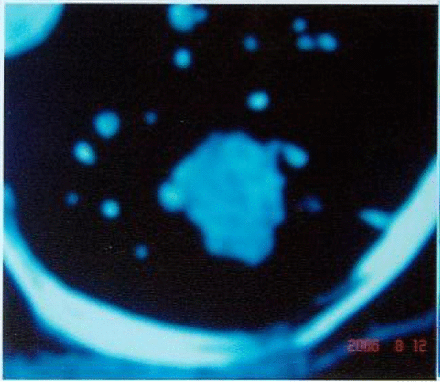
One month after treatment of the same case
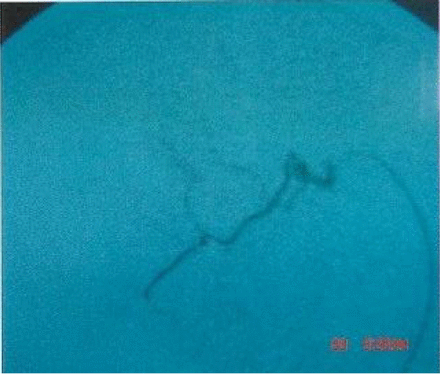
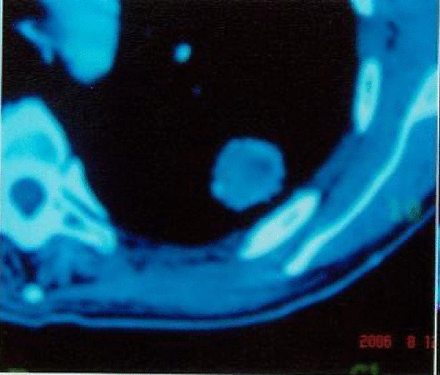
Three months after treatment of the same case
Safety and efficacy have always been stressed in tumor therapy, with a goal of minimal toxicity. Targeted therapy for lung cancer angiogenesis includes two main approaches, i.e. the first method is to target the lung cancer vessels and the second is to inhibit angiogenesis. Angiogenesis is necessary when tumor cells move into the blood vessels and even the lymphatics, and it also supplies oxygen and nutrients for continuous growth of the metastasized sub-foci[6]. The character of the new tumor vessels can be used in imaging targeted therapy, in which the embolizing agents and the regional chemotherapeutics are selectively sent into tumors via the blood vessel at a high flow rate[7,8]. Bronchial arterial catheter chemotherapy and embolotherapy can supply a plasma drug concentration which is six or even ten times higher compared to an i.v. infusion. At the same time, it has an effect on antiangiogenesis, with little unwanted drug metabolism, a minimal whole-body toxic effects, a short duration and rapid efficacy. The inhibition of angiogenesis can depress growth of the lung cancer cells, enhance apoptosis and restrain migration of the tumor cells. Using trascatheter chemotherapy and embolotherapy with our 56 patients resulted in complete remission in 88.9% (8/9) of the SCLC cases and in 78.7% (37/47) of the NSCLC cases (Figs.5~11).
New vessels of a poorly-differentiated adenocarcinoma
DSA image before treatment of the same case
DSA image 1 month after treatment of the same case
Peripheral new vessels of a moderately differentiated squamous cell carcinoma in the left thorax
Image of the blood-flow perfusion in the tumor of the same case
Peripheral abnormal arteriola and central stamen’s sign of the moderately differentiated adenocarcinoma in the left thorax
The image of blood-flow perfusion in the tumor of the same case.
The therapeutic dose of the drugs, reaching the large tumors by the blood circulation, was less compared to the small tumors, and it supplied the basis for targeted therapy of imaging of the metastatic lesions. Whole-body treatment is difficult for large tumors, because the tumor mesenchymal pressure is high and diffusion speed of the therapeutic agent is slow, making it hard to reach a large tumor. Radiotherapy can reduce the mesenchymal pressure in solid tumors, increase the blood flow and improve uptake of antibodies and other macromolecules. In the group of 26 lung cancer patients to which 5,000 to 7,000 Gy of radiotherapy was added during the interventional therapy, the curative effect was significantly improved.
With further understanding of tumor biology, such as the growth, differentiation and apoptosis, targeted therapy for lung cancer will take on more importance. The arterial interventional therapy can be used for selection of target organs for gene therapy, to monitor and detect uptake of genes and their expression in the target tissue, as well as to observe the clinical reaction, etc.[9] The results of our study indicated that higher malignancy was associated with richer angiogenesis and better short-term curative effects of interventional therapy. In some cases, the clinical stage was decreased, even with complete remission. Further follow-up visit and summary of the long-term effect will be conducted in the future.
Our study of lung cancer angiogenesis using imaging technology improves the therapeutic efficacy. Embolizing agents for interventional therapy, large doses of anti-tumor drugs and angiogenesis inhibitors were selectively delivered into the tumor vessels. This modality of therapy can eliminate the primary tumor, and thereby decrease tumor metastases and thus enhance the curative effect of the therapy.
- Received December 5, 2006.
- Accepted December 29, 2006.
- Copyright © 2007 by Tianjin Medical University Cancer Institute & Hospital and Springer