Abstract
OBJECTIVE To investigate the effect of intermittent androgen blockade (IAB) on the quality of life (QOL) of patients with advanced prostatic carcinoma (APC).
METHODS Investigations on the QOL of 51 APC patients receiving IAB treatment, totaling 3 times, i.e. 6 months before and after, and 12 months after treatment, were perform using the EORTC QLQ-C30 measuring scale and QLQ-PR25 scale.
RESULTS Although IAB became an economic burden for the families, it was lessened during the intermission (P<0.05). The overall health status significantly improved 6 months after IAB treatment (P<0.01), especially during the intermission (P<0.05), with a total or local easement of pain (P<0.01) and an improvement of urinary function (P<0.01). Although there was impairment, to various degrees, in many functions of the patients on the 6th month of treatment, such as the physical function (P<0.05), role function (P<0.05), the emotional (P<0.01) and the social functions (P<0.01), with an enhancement of fatigue (P<0.01), these functions gradually recovered by the 12th month as the intermission started. Treatment-related symptoms such as flushing and mammary swelling significantly emerged on the 6th treatment month (P<0.01), and lessened on the 12th (P<0.01). During the treatment period, there was an notable drop in sexual interest (P<0.01), with a deprivation of sex life, but revived to various degrees during the intermission (P<0.01).
CONCLUSION Although IAB treatment of APC patients did impair the physiologic and psychologic status of patients to varying degrees, these were improved and restored during the intermission.
keywords
INTRODUCTION
With changes in the ecological environment and life style, there is a year-by-year rising tendency in the incidence of prostatic carcinoma (PC) in China. Because of a relative backwardness in the economic conditions and level of medical detection in China, advanced prostatic carcinoma (APC) ranks first now in the incidence of clinical cases[1]. Based on an androgen dependence of most PC cases, endocrine castration therapy has become the treatment of choice for APC patients. Since 2000, intermittent androgen blockade (IAB) for APC has made definite progress in our hospital[2]. The report on the quality of life (QOL) of APC patients before and after IAB treatment follows.
MATERIALS AND METHODS
Clinical data
From October 2004 to April 2007, a final pathologic diagnosis of all 51 APC patients was made. The mean age of the patients was 71±8 years. Before treatment, a value of serum PSA<10 ng/ml was found in 3 cases, that of PSA=10~100 ng/ml in 18 and PSA>100 ng/ml in 30. Of the 51 cases, there were 5 at Stage-T3, 13 at Stage-T4 and 33 with bone metastases. A Gleason score of ≤6 was determined in 19 cases, and the score of ≥7 in 32. Goserelin, an analogue of luteinizing hormone-releasing hormone (LHRH), plus antiandrogen drugs such as flutamide or bicalutamide were continuously administered until the PSA serum value was <0.2 ng/ml. Then a 3-month maintenance therapy was conducted before the drugs were withdrawn. An intermission started after the discontinuation of the treatment.
EORTC QOL questionaire (QLQ-C30+ QLQ-PR25)
The European Organization for Research on Treatment of Cancer (EORTC) which devised the QLQ-C30 measuring scale for the QOL of cancer patients[3], is comprised of 30 items. It includes the following 5 functional scales: a physical function (PF), role function (RF), cognitive function (CF), emotional function (EF) and social function (SF); 3 symptom scales: fatigue (FA), pain (PA), nausea and vomiting (NV), 6 individual items: dyspnoea (DY), insomnia or sleep disorder (SD), loss of appetite (LA), constipation (CO), diarrhea (DI), financial straits or financial difficulties (FD), and a global QOL questionaire (Global QLQ).
In the scales described above, the higher the score of a functional scale, the better the state of the patient’s QOL. However, the higher the score of a symptom scale, the poorer the state of the patient’s QOL. A classification scoring method was employed in assessment of the questionaire’s indices, and the global health (GH) status or QOL was divided into 7 levels, i.e. numbers from 1 to 7. The scores for other indices were divided into 4 levels, from 1 to 4 scores. The rater was requested to have in mind the patient’s general status 7 days before the scoring was conducted. After a linear conversion, a solitary scoring of the 5 function items and GH scale was calculated using the same method, and the score of all the individual items fluctuated in a range between 0 and 100, with a high score representing a high functional level. Solitary scorings of the symptom scales with multiple and singular index were also conducted respectively, with a scale mode of 0~100, after the linear conversion, by which a high score represents a severer symptom or problem.
The QLQ-PR25 is a scale for the QOL for PC patients (supplied by Karen West, EORTC QOL Group) comprised of 25 items, including 3 symptom scales and 1 sexual function scale: urination symptoms, bowel symptoms, treatment-related symptoms and sexual function. The sexual-function scale was divided into 3 parts: sexual desire, sexual delight and the quality of sexual life. The calculation method of the PR25 scales was as follows, i.e. the symptom scale: S=|(RS-1)/range}×100; the sexual desire and sexual delight in the sexual function scale: S=|(RS-1)/range}×100; and the quality of sexual life: S=|1-(RS-1)/range}×100, in which RS = (I1+I2+I3+...+In)/n. The scores of the function and symptom scales were the poorest (range), i.e. 3. In these scales, the higher the score of the functional scale, the better the state of the patient’s QOL, but the higher the score of the symptom scale, the poorer the state of the patient’s QOL. Specific calculating method was the same as the QLQ-C30.
Methods ascertaining the QOL
In April 2006, the EORTC QLQ-C30+QLQ-PR25 was utilized for the patients followed-up, and the QOL determined at 3 appraisement points, i.e. 6 months before and after treatment, and 12 months after treatment. Some patients were provided with 2 or 3 questionaires for assessing their QOL 6 months before and after treatment, and 12 months after treatment. Since loss of follow-up and progression of diseases (PD) occurred in part of the patients, the total 3 questonaires could not be completed. The PD includes clinical progression (extension of the metastasis or occurrence of new metastasis) and biochemical progression (the blood testosterone had attained the level of castration during the IAB therapy, while serum PSA was still continuously rising). Results of completion of the questionaire can be seen in Table 1.
Completion of the questionaire.
For the outcome of QOL of the APC patients treated with IAB (QLQ-C30 and QLQ-PR25) (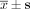 ), see Tables 2 and 3.
), see Tables 2 and 3.
The scoring of the QLQ-C30 scale (100 scores).
Scoring of the QLQ-PR25 scale (100 scores).
Statistical analysis
The multiple-comparison q test (Newman-Keuls method) or t test among the mono-factorial and multisample means was used to conduct the statistical analysis for the scoring value of these appraisal points. A P<0.05 was considered to be statistically significant.
RESULTS
Of the 51 patients, 41 (80.4%) patients completed 3 questionaires, and 2 questionaires were completed by 45 (88.2%) patients. The average IAB treatment period was 7.3±2.9 months, and 44 of the total patients received surgical treatment at the 6th month following IAB. At the 12th month after surgery the intermission started for the 41 patients who had completed 3 questionaires. Results of the EORTC QLQ-C30+QLQ-PR25 showed that although the IAB brought about more financial burden for the patient’s families (P<0.05), the burden was alleviated during the intermission (P<0.05). Six months after the IAB treatment, the GH status of the patients significantly improved (P<0.01), which was especially notable during the intermission (P<0.05), with a relief of systemic or regional pain (P<0.01) and with improvement in urinary symptoms (P<0.01). At the 6th month following the surgical treatment, the patient’s functions, such as the physical function (P<0.05), role function (P<0.05), emotional (P<0.01) and social functions (P<0.01) etc. decreased in varying degrees, with increased fatigue (P<0.01), however, these functions gradually restored at 12 months after surgery when the intermission began. There was a prominent emergence of treatment-related symptoms such as flushing and mammary swelling and pain etc. at the 6th month (P<0.01), but these symptoms were significantly alleviated by the 12th month (P<0.01). Sexual desire markedly decreased during the treatment period (P<0.01), with a deprivation of sex life. Nevertheless recovery was made in varying degrees during the intermission (P< 0.01).
DISCUSSION
Since the discovery of the hormonal dependence of PC by Huggins in 1941, thus paving the way for PC endocrine therapy, endocrine castration (EC) has been the treatment of choice for APC. Over the past few years, the view of IAB therapy gradually became the mainstream mode of treatment[4]. The theoretical foundation of the therapy is to maintain the sensitivity of the tumor to the androgen inhibition by intermittent administration, and thus delay the hyperplasia and progression of non-hormonal dependent PC cells. This treatment has the advantage of prolonging the survival time compared to continuous androgen blockade (CAB) used in the past, thus improving the QOL, such as restoration of sexual desire and function, decreasing treatment-related side effects and reducing medical costs etc. It was suggested by Yu et al.[2] after a 5-year clinical follow-up, that EC treatment by androgen blockage was the preferred therapy for APC patients.
Owing to the nature of advanced cancer patients, to enhance the patient’s QOL has become the main goal of advanced cancer treatment. So application of QOL scoring attempts to appraise the therapeutic efficacy and GH status of the patients.[5] For instance, Shen and Zhang[6] and Zhao et al.[7] have employed the Karnofsky performance status scale (KPSC) to assess the QOL of advanced malignant tumor patients, suggesting that the KPSC was a good means to appraise the QOL of cancer patients. Although the KPSC can be used to determine the commonality of the QOL of all cancer patients, since the KPSC is merely a general QOL scale, there is a definite flaw in appraising the clinical manifestations of specific cancers. The EORTC QLQ-C30 and QLQ-PR25 scales, as specific measuring scales for assessing the QOL of PC patients, have been adopted in clinical research on PC since 2002. For example, Wahlgren et al.[8] and Buron et al.[9] used the QLQ-C30 and QLQ-PR25 to compare the effects of external and internal irradiation, and PC radical surgery on the QOL. They indicated that the QLQ-C30 and QLQ-PR25 scales are the preferred scoring means for measuring the PC patient’s QOL. Voerman et al.[10] suggested that QLQ-C30 and QLQ-PR25 have a very high specificity in assessing the QOL of PC patients. In our study, the EORTC QLQ-C30 and QLQ-PR25 scales were used to appraise QOL of the APC patients in the Wenzhou prefecture.
Herr and O’Sullivan[11] and Moinpour et al.[12] reported that castration had both physical and mental effects of different degrees on the PC patients. Our study showed that IAB can significantly improve the patient’s GH status (P<0.01), and lessen the clinical symptoms, such as pain (P<0.01), frequent micturition and urgency (P<0.01), etc. Although the negative effects of the therapy were notable, e.g., lessened activity in social functions (P<0.05), limitation of routine work and daily activities (P<0.05), with a fluctuation of emotion (P<0.01), frequent restlessness and anxiety as well as fatigue (P<0.01), these symptoms ameliorated and the functions gradually were restored when intermission started. The castrationrelated symptoms such as flushing, mammary swelling and pain, and edema of the lower limbs, etc. were also alleviated during the intermission.
A decrease in sexual function was the major side effect of the IAB treatment. Our study showed that IAB therapy results in a significant decrease in sexual desire in most patients (P<0.01), resulting in a deprivation of sex life. However, the symptoms were improved to varying degrees at the initiation of the intermission (P<0.01). Therefore it is necessary to explain to the patients the effects on sexual function with IAB treatment before treatment begins.
In conclusion, extension of the survival time of the APC patients and reduction of the effect of IAB on the QOL should be the goal in treating APC patients. In view of a rather short follow-up period of the patient QOL (3~20 months), and because of the small number of cases in this study, a multi-central, large-scale, long-term analysis of the APC patients is needed to thoroughly appraise the applied value of IAB therapy.
- Received August 17, 2007.
- Accepted October 31, 2007.
- Copyright © 2007 by Tianjin Medical University Cancer Institute & Hospital and Springer











