Abstract
OBJECTIVE Pegylated liposomal doxorubicin (PLD; CAELYX®), a novel formulation of doxorubicin with enhanced therapeutic efficacy and reduced toxicity, has demonstrated improved progression-free survival in recurrent or refractory ovarian cancer. The objective of this open-label, non-comparative, observational study was to determine the efficacy and safety of PLD monotherapy or combination therapy with carboplatin for patients with recurrent or refractory ovarian cancer.
METHODS Sixty-two patients with recurrent or refractory ovarian cancer who completed a platinum-based chemotherapy regimen and demonstrated platinum sensitivity for first-line treatment at least 6 months prior to study entry were enrolled in 20 centers in China. PLD was given as monotherapy (50 mg/m2 infused over 60 minutes) or as combination therapy (30 mg/m2 1-hour infusion) with carboplatin (area under the curve 5 mg·min/mL 1-hour infusion) on day 1 every 28 days for 4 cycles. The primary endpoint was objective response (OR) rate or CA-125 level. Secondary endpoints included time to response, time-to-progression, health-related quality of life, and safety.
RESULTS Overall, 48% of the 62 evaluable patients achieved a confirmed OR. More patients receiving PLD and carboplatin achieved an OR vs the PLD monotherapy group (63% vs. 37%). The median time to response and disease progression was 58.5 days and 56.0 days, respectively. Overall and drug-related adverse events were reported for 39% and 34%, respectively. The most commonly reported adverse events were stomatitis (22.6%) and palmar-plantar erythroderma (9.7%). Two deaths were reported.
CONCLUSION PLD is an effective and well tolerated agent in women with recurrent or refractory epithelial ovarian cancer.
keywords
Introduction
Delays in diagnosis, due to lack of recognition of common symptoms such as abdominal pain and swelling, gastrointestinal symptoms, and pelvic pain, can contribute to the occurrence of widespread ovarian cancer at diagnosis[1-3]. Ovarian cancer ranks fifth in cancer deaths among women[4]. The 1-year survival rate after diagnosis is approximately 76%, and 45% survive longer than 5 years after diagnosis.
Recommended primary or adjuvant therapy for ovarian cancer is a combination of surgical staging and cytoreduction plus 3 to 6 cycles of cytotoxic therapy with a taxane and a platinum compound (eg, carboplatin, oxaliplatin, or cisplatin), although alternative regimens are available[5]. The prognosis in these patients is poor if they progress after 2 consecutive chemotherapy regimens without a clinical benefit or for those whose disease recurs in less than 6 months. In general, retreatment with a platinum compound or paclitaxel is not recommended, because of resistance to the primary induction regimen[5]. Evidence suggests that a non-platinum-based regimen may be efficacious. For patients who cannot tolerate or have had unsuccessful results from chemotherapy regimens, hormonal therapy with tamoxifen or other aromatase inhibitors may be considered.
Patients who relapse more than 6 months after initial chemotherapy are considered “platinum-sensitive” and have the greatest number of potential options for second-line therapy. In selected patients, there are potential ancillary surgical and/or supportive care procedure options. Evidence suggests that platinum-based combination chemotherapy may be superior to single-agent therapy in this situation[6]. Overall response rates reported with several newer cytotoxic agents in ovarian cancer appear similar as follows: topotecan, 20%[7]; gemcitabine, 19%[8]; vinorelbine, 20%[9,10]; liposomal doxorubicin, 26%[11]; and oral etoposide, 27% in platinum-resistant patients and 35% in platinum-sensitive patients[12]. While the aims of treatment for recurrent or resistant disease traditionally have been palliative, the introduction of pegylated liposomal doxorubicin (PLD) (Caelyx®, Schering-Plough Corporation, Kenilworth, NJ), has demonstrated the ability to increase progression-free survival[13]. One option includes the use of PLD alone or in combination with a platinum-based therapy in patients whose ovarian cancer recurs after 6 months, because these patients are considered platinum-sensitive.
Pegylated liposomal doxorubicin (PLD) is a unique formulation of doxorubicin in which a polyethylene glycol layer surrounds a doxorubicin-containing STEALTH ® liposome. The purpose of pegylation is to protect the liposomes from detection and breakdown by the reticuloendothelial system[14]. The protective coat of the drug increases the plasma half-life compared with conventional doxorubicin, thus the drug stays longer in circulation similar to a prolonged infusion. This formulation also allows the drug to penetrate through defective tumor vessels as an intact liposome, accumulating drug in the tumor tissue over a prolonged period[15]. The purpose of this study was to determine the efficacy and safety profiles of PLD as a single agent or as combination therapy with carboplatin for patients with recurrent or refractory ovarian cancer.
Patients and Methods
Study design
This open-label, non-comparative, observational, multicenter study evaluated the safety and efficacy of monotherapy of PLD or combination therapy with carboplatin and PLD. Adult patients with recurrent or refractory ovarian cancer from 20 centers in China were evaluated. This observational study was conducted in conformance with Good Clinical Practices.
Eligibility criteria
Eligible patients were women who were ≥ 18 years old and had histologically proven ovarian epithelial cancer that was documented as recurrent or refractory by appropriate radiologic imaging (such as, X-ray, ultrasound, CT scan, MRI) with measurable or evaluable disease. Evaluable disease was defined as unidimensionally measurable lesions, masses with margins not clearly defined, lesions with both diameters ≤ 0.5 cm, lesions on scan with either diameter smaller than the distance between cuts, palpable lesions with either diameter ≤ 2 cm, or bone disease. Patients should not have received prior treatment with PLD, and for combination therapy, should have completed a platinum-based chemotherapy regimen and demonstrated platinum sensitivity for first-line treatment at least 6 months prior to study entry.
In addition, patients must have an Eastern Cooperative Oncology Group (ECOG) performance status ≤ 2; normal electrocardiography; normal organ function, except if abnormal due to tumor involvement; bone marrow function (platelets > 100,000/mm3, hemoglobin > 10 g/dL, and neutrophils > 1.5 × 103/mm3); renal function (serum creatinine < 2.5 mg/dL); and liver function (serum bilirubin and transaminase levels > 2 × upper limit of normal). Written informed consent was obtained from all patients.
Patients were excluded from the study if they had non-evaluable disease, which was defined as pleural effusions, ascites, or disease documented by indirect evidence only, such as by a laboratory value. In addition, patients were excluded if they had received PLD for treatment of a gynecologic malignancy, hypersensitivity to anthracycline therapy, prior radiation therapy to more than 1/3 of the hematopoietic sites, or had symptomatic metastasis to the brain. Other exclusion criteria were a history of cardiac disease (congestive heart failure); clinically significant hepatic disease; uncontrolled bacterial, viral, or fungal infection; pregnant or breast feeding; exhibited confusion or disorientation; any other active primary tumor, under treatment, except basal or squamous cell carcinoma of the skin or carcinoma in situ; or any condition (medical, social, and psychosocial) that would prevent adequate follow-up.
Treatment plan
PLD was given as a single agent (50 mg/m2 infused over 60 minutes) or as combination therapy (30 mg/m2 infused over 60 minutes) with carboplatin at area-under-the-curve (AUC) (5 mg·min/mL1-hour infusion) on day 1 every 28 days for 4 cycles. Patients with disease recurrence at least > 6 months from prior platinum-based therapy (platinum-sensitive disease) were included in the combination therapy group. Patients without platinum-sensitive disease were included in the single-agent group. Drug dosage was modified as a function of hematologic nadir or when the patient was unable to tolerate the dose. Patients were premedicated with antiemetics, 5-hydroxytryptamine 3 (5-HT3) receptor antagonists, prior to receiving carboplatin, and were properly hydrated as per the protocol for carboplatin infusion.
Treatment discontinuation was allowed if the patient developed progressive disease or was unable to tolerate the therapy despite dose reduction. In addition, treatment was discontinued for an absolute granulocyte count < 500 cells/mm3 for 3 consecutive cycles after dose reduction or other grade 4 hematologic toxicities, excluding anemia or any grade 4 nonhematologic toxicity. Patients were also excluded if they had a clinical need for concomitant drugs contraindicated by the protocol, exhibited signs and symptoms of cardiotoxicity, if the physician had concern related to the patient’s welfare, or if the patient withdrew consent.
If patients required palliative or primary radiation therapy, study drugs were withheld during the course of radiation therapy until recovery. The suggested minimum time was at least 30 days after radiation. These patients were retreated with study drug provided that the metastases did not represent progression of disease and there was no evidence of radiation recall reaction.
Efficacy assessment
The evaluable patient population for the primary efficacy analysis included all patients who met all inclusion and exclusion criteria, received at least 2 cycles of study drug as prescribed, and completed all visits according to the study schedule. All patients who received at least one dose of study drug (partial or complete dose) were included in the intent to treat (ITT) analyses. The primary endpoint was an objective response (OR) rate, including complete response (CR: complete disappearance of all measurable and evaluable disease) and partial response (PR: 50% decrease in the sum of the products of bidimensional perpendicular diameters of all measurable lesions), as determined by physical examination and radiological assessments, or tumor marker (CA-125 level). Radiological imaging (i.e., X-ray, CT scan, MRI, or ultrasound), CA-125 levels, and objective response rates were obtained prior to the study, after every 2 cycles, and at the end of the study. Patients who achieved a CR or PR were reevaluated every 4 weeks afterwards to confirm the initial observation of response. Secondary endpoints included time to response (time from the start of study drug to the first observation of durable response), time to progression (time from the first observation of durable response to the first observation of progressive disease, or to death due to any cause, or early discontinuation of treatment due to progressive disease), and health-related quality of life (HR-QOL). The European Organization for Research and Treatment (EORTC) core quality of life questionnaire (QLQ-C30, version 3.0) was completed at baseline and at visits 1-4. The questionnaire was designed to measure cancer patients’ physical, psychological, and social functions and is composed of 5 multi-item scales (physical, role, social, emotional and cognitive functioning) and 9 single items (pain, fatigue, financial impact, appetite loss, nausea/vomiting, diarrhea, constipation, sleep disturbance and quality of life).
Safety assessments
All patients who received at least one dose of study drug (partial or complete dose) were evaluable for safety. Safety was assessed by examination of adverse events, clinical laboratory data, and vital signs prior to study (baseline), prior to each cycle, and at the end of the study. Adverse events were recorded during the treatment, which included details such as symptoms, duration, severity and correlation (no-correlation, possibly no-correlation, possible correlation, and correlation), measures, and corrections. Severe adverse reactions were assessed as those reactions that prolonged in-hospital time, or when there was danger of life, severe or lasting disability, occurrence of cancer, or overdose (dose more than permitted intentionally or not). In addition, cardiac safety assessments were evaluated: in the event of decreasing cardiac function, treatment was continued if there was evidence of clinical benefit and if cardiac biopsy demonstrated no evidence of cardiac damage.
Statistical analysis
Continuous variables were summarized by mean, median, standard deviation and range. Categorical variables were summarized by frequency and percentage. The objective response rate was calculated and reported along with the two-sided 95% confidence interval. Time to response and time to progression were summarized. EORTC QLQ-C30 score was summarized at each visit, and the changes from baseline were also concluded along with two-sided 95% confidence interval. Treatment emerging events (AEs) were summarized. AE severity and their relationship to the study medication would also be presented. The number of patients reporting any AEs, the occurrence of specific AEs, and discontinuation due to AEs would be tabulated. SAS 8.02 was used to analyze the data.
Results
A total of 62 patients were enrolled in the study and received treatment (Table 1). The mean age was approximately 53 years, and the mean of duration of disease was 2.8 years. Of these patients, approximately 90% were enrolled because of evaluable disease, whereas, approximately 10% of patients were enrolled with a CA-125 level increase alone. The majority (53%) of patients had grade IIIc disease and 13% had grade IV disease. Overall, 56% of patients had an ECOG score of 0, 35% of patients had an ECOG score of 1, and 6% of patients had an ECOG score of 2. Among the 62 patients, 35 were treated by PLD single agent therapy and 27 were treated by combination therapy.
Patient demographics.
Efficacy
The intention-to-treat efficacy analysis was based on 62 patients; a confirmed OR was achieved in 48.4%. When evaluating each treatment arm, more patients with carboplatin and PLD combination therapy achieved an OR (63%) compared with the PLD monotherapy group (37%) (Table 2). The CR rate was 14.3% and 25.9%, and the PR rate was 22.7% and 37.0% for monotherapy and carboplatin combination therapy groups, respectively. Overall, 19.4% of patients had stable disease, defined as those that did not qualify for CR, PR, or progression, and 25.8% of patients had progressive disease, defined as a greater than 25% increase in the sum of the products of the longest perpendicular diameters of lesions or the appearance of new lesions.
Response rates with PLD monotherapy or plus carboplatin.
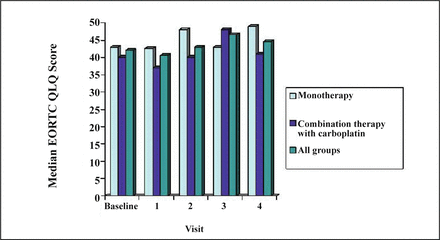
The overall median time to response was 58.5 days (54 days for monotherapy and 62 days for combination therapy), and the median time to progression was 56.0 days (52 days for monotherapy and 75 days for combination therapy). Results of the EORTC QLQ-C30 (Fig. 1) showed that there were no consistent changes or significant differences in the overall health-related quality of life in either treatment group or the combined group over time.
Median EORTC QLQ score at baseline and at visits 1, 2, 3, and 4 for each treatment group. There were no consistent changes or significant differences in the overall health-related quality of life in either treatment group or in the combined group over time.
Safety
Overall, 24 (38.7%) patients reported adverse events. Two patients in the PLD-monotherapy arm (n = 35; 5.7%) experienced drug-related death. The most commonly reported adverse events related with PLD were stomatitis (22.6%), palmar-pantar erythrodysesthesia (PPE: 9.7%), diarrhea (3.2%), and stomach ache (3.2%) (Table 3). Stomatitis, diarrhea, and stomach ache were seen more frequently in the PLD-monotherapy arm compared to the PLD combination with carboplatin arm. The dose-limiting toxicity of PLD was PPE. These adverse reactions were assessed carefully prior to administration of each cycle. Increasing the length of the cycle was the optimum method for avoiding subsequent occurrence of the PPE.
Adverse events (AEs) in patients receiving PLD monotherapy or combination of PLD and carboplatin.
Serious events occurring most frequently with carboplatin were bone marrow suppression, peripheral neuropathy, and renal toxicity. After a total of 4 cycles the study physician decided if the patient should continue therapy with PLD or other drugs. Severe hypersensitivity reactions required immediate discontinuation and appropriate therapy, and patients such as these were not rechallenged.
Discussion
First-line treatment options for advanced ovarian cancer such as carboplatin and paclitaxel are typically associated with resistance or refractoriness. A different agent is warranted (e.g., second-line) based on delayed diminution in computerized tomography scan measurements after the second and the fourth treatment cycles. PLD may be used in the second-line treatment setting, either as monotherapy or in combination in platinum-sensitive patients.
Though conventional doxorubicin has a widespread degree of clinical use in the adjuvant setting for endometrial cancer, ovarian, and cervical cancer, its associated toxicity may preclude adequate dosing, thus limiting its potential therapeutic effect. The potential for cardiotoxicity is associated with high cumulative doses of doxorubicin, while individual doses are often limited by myelosuppression. Because of its toxicity profile, its use either as a single agent or as part of a combination regimen is limited.
Caelyx®, a novel liposomal formulation of doxorubicin, was developed to maintain the anti-tumor activity of doxorubicin by delivering doxorubicin to tumors with improved specificity. In addition, decreased toxicity is generally seen due to a reduction in nonspecific drug delivery to normal tissues and the high peak plasma levels of free drug, which are responsible for toxicity. Tumor-selective uptake has been observed in patients whose lesions could be biopsied in early clinical trials[16]. Doxorubicin levels were observed in the lesions of 18 patients with AIDS-related Kaposi’s sarcoma receiving PLD that were 5.2 to 11.4 times greater than those found in the patients receiving comparable doses of standard doxorubicin.
The STEALTH® liposomes evade recognition by the immune system because of their unique PEG coating, which avoids the rapid hepatic uptake characteristic of conventional liposomes and has been documented to have a circulation half-life in man of 40 hours, which is approximately 100-fold longer when compared to standard doxorubicin. Following PLD administration, the time to neutrophil count (ANC) nadir is also extended relative to standard doxorubicin (approximately 21 days for PLD compared to 10 to 14 days for doxorubicin).
Data from this study show that PLD was generally well tolerated. Drug-related adverse events were reported in 34.3% of the monotherapy group and 33.3% of the carboplatin combination therapy group, demonstrating tolerability. Indeed, the tolerability of PLD in relapsed ovarian cancer has been demonstrated in a number of phase II and III studies[11,13,17,18]. One of the most common adverse events associated with PLD is PPE[11,13,17,18]. PPE, which is also called hand-foot syndrome, presents as a cutaneous reaction typically involving the soles of the feet and palms of the hands. The reaction begins with paresthesias of the extremities that is followed by erythema and edema, sometimes complicated by severe pain and cracking of the skin. The exact cause of PPE is unknown; however, the pharmacokinetics and size of the liposomes may result in localization of PLD in the skin. Early recognition of PPE symptoms is important in the management of this adverse event. Dose modification, by decreasing the dose or lengthening the dosing interval, has been recommended and is effective in preventing or reducing toxicity[13,19]. Patients can also minimize the reaction by avoiding those daily activities that cause increased perfusion of the skin or mild trauma to skin surfaces.
In this study, patients had not received prior treatment with PLD and for combination therapy, should have completed a platinum-based chemotherapy regimen and demonstrated platinum sensitivity for first-line treatment at least 6 months prior to study entry. Overall, 48.4% of the 62 evaluable patients achieved a confirmed OR. The CR rate was 14.3% and 25.9% and the PR rate was 22.7% and 37.0% for monotherapy and carboplatin combination therapy groups, respectively.
The efficacy of PLD in relapsed ovarian cancer has also been demonstrated in phase II and III studies[11,13,17,18]. For example, phase II studies by Muggia et al.[11] and Gordon et al.[17] showed response rates of 26% and 17%, respectively, for relapsed ovarian cancer. A phase III trial compared the use of PLD versus topotecan as second-line treatment for platinum/paclitaxel-resistant ovarian cancer, demonstrating comparable efficacy and favorable tolerability profile for PLD[13]. The overall response rates for PLD and topotecan were 19.7% and 17.0%, respectively (P = 0.390), and the median progression-free survival rates were 28.9 and 23.3 weeks, respectively (P = 0.037). Long-term follow demonstrated that PLD significantly prolonged survival compared with topotecan, and the survival benefit was marked in patients with platinum-sensitive disease[18].
Recently reported results of a randomized phase III trial, CALYPSO, demonstrated the advantage of the PLD-carboplatin combination over the standard paclitaxel-carboplatin combination in 976 patients with recurrent ovarian cancer relapsing > 6 months after first- or second-line platinum-based therapy[20]. The median progression-free survival (the primary endpoint) was significantly superior in the PLD-carboplatin arm versus the paclitaxel-carboplatin arm (11.3 vs. 9.4 months, P = 0.005). Notably, premature discontinuation of therapy due to toxicity was more frequent in the paclitaxel-carboplatin arm (15% vs. 7%) as were non-hematologic grade 3-4 toxicities (37% vs. 28%). These results demonstrate PLD-carboplatin to be a viable treatment option for women with platinum-sensitive recurrent ovarian cancer.
In summary, PLD has a convenient administration schedule, making it an ideal agent to administer in an outpatient clinic. Because of its favorable toxicity profile, PLD can be administered every 21-28 days, maximizing delivery of doses and therapeutic effect. In this trial, PLD was effective and well tolerated in women with recurrent or refractory epithelia ovarian cancer.
Acknowledgements
We would like to acknowledge The Phillips Group for technical assistance with this manuscript. Schering-Plough provided the study drug-Caelyx, and the research grant.
- Received September 21, 2009.
- Accepted November 24, 2009.
- Copyright © 2009 by Tianjin Medical University Cancer Institute & Hospital and Springer