Abstract
OBJECTIVE To study the clinical pathologic characteristics and differential diagnosis of ureteral fibroepithelial polyps.
METHODS One case of ureteral fibroepithelial polyps was studied by clinical data analysis and light microscopy.
RESULTS The tumor was located in the lower ureter. Histologically, the polyp was composed of expanded blood vessels and fibrous connective tissue under normal or proliferous transitional epithelium.
CONCLUSION Benign ureteral fibroepithelial polyps are extremely rare, recognition of it's precise histological features can facilitate its correct diagnosis.
keywords
Ureteral fibroepithelial polyps (FEP) are rare benign tumors, which are usually encountered in children, but are especially un-common in adults. This article is a report of a case of ureteral fibroepithelial polyps in an adult. We have summarized its pathogenesis, pathologic characteristics and differential diagnosis from relevant reports.
Case Report
A 40-year-old man presented with a ureteral mass to the Second Affiliated Hospital of the General Hospital of the PLA, Beijing, China. It was detected incidentally in a general health examination. Physical examination of the patient was unremarkable, with no indication of hematuria, frequent micturition, urgent micturition, pain during urination or dysuria. B-mode ultrasound showed a 2.3 × 1.6 × 0.8 cm tumor in the posterior wall of the bladder. Intravenous pyelography and nuclear magnetic resonance both indicated that the tumor was in the lower left ureteral segment. At surgery, there was a palpable dilation 5 cm distal to the left ureteropelvic junction, and a slight dilatation of the upper ureter. In addition, the ureter wall was thicker than normal. A longitudinal ureterotomy incision was made and a mass with smooth surface approximately 0.8 cm in width was encountered. The pelviureteric region, including the polyp, was resected segmentally and then was sent for histopathologic examination.
General biopsy
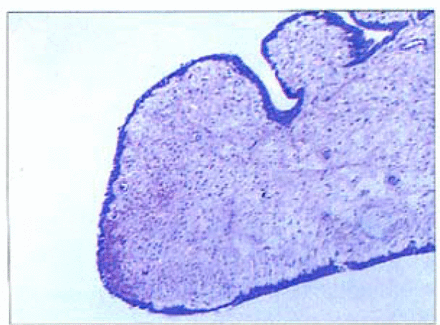
A pale polyp-like mass with a smooth surface was encountered in the lower ureter, it was 7 cm long and 2 cm wide with a diameter of 1 cm. Microscopically, the polyps were covered by a benign-appearing transitional cell epithelium supported by a loose, vascular connective tissue infiltrated by lymphocytes (Fig. 1). The final pathologic diagnosis was conformed to be left ureteral fibroepithelial polyps.
Vascular loose fibrous stroma of the ureteral fibroepithelial polyps covered by transitional epithelium (H&E staining × 40).
DISCUSSION
Ureteral fibroepithelial polyps are uncommon benign tumors, which are usually encountered in children, but are rare in adults[1]. Incidence of this disease is quite low, with a projection that primary ureteral tumors comprise only 1/3,690 of the total number of urology patients. Most ureteral tumors are malignant, and benign tumors only constitute 1/20 of the total number[2]. But the actual incidence must be higher than that reported, as many cases may be completely asymptomatic for many years. Ureteral fibroepithelial polyps are a non-epithelial tumor[3], but other authors suggest that they are a tumor-like hyperplasia. In spite of the theory, which has little clinical relevance, it is well known that ureteral fibroepithelial polyps are benign tumors.
Pathogenesis
The exact etiology of the polyps is not certain. Many theories have been proposed including congenital obstruction, trauma, irritation, infection, and allergic factors[4]. Downs [5] speculated that fibroepithelial polyps originate from developmental defects of the urinary tract, while Kuppusami and Moors [6] attributed the pathogenesis to the absence of estrogen in the matrix and subsequent fibroepithelium transformation, Lou et al[7]. have suggested that FEP polyps derive from congenital malformation, an etiology being the most frequently accepted.
Patients may either be completely asymptomatic or present with unrelated symptoms, suggesting that the tumor cannot be related to a single origin. We believe that more than one factor is involved during the development of this disease.
Clinical symptoms
Clinical symptoms of fibroepithelial polyps frequently appear between the second and fourth decades of life, although the polyps can occur at any age [8]. Macksood et al[9]. hold that fibroepithelial polyps are the most usual benign ureteral lesion in children. In adults, the majority of these tumors are seen in the upper ureter, at the ureteropelvic junction[10]. There is no notable incidence difference between the left and right sides and no familial traits have been reported.
Flank pain and hematuria are the leading symptoms, but infection, urgent maturation, dysuria and urinary tract obstruction also occur as familiar symptoms. As some noted previously, cases remain completely asymptomatic for many years, until the development of hydronephrosis, which is related to the degree of obstruction of the ureter. Such was the patient's condition in our case.
In general, calcului can be found occasionally as a complication and will be not implanted into the urinary tract without growing obviously thick. However, FEP initiated by calcului are rarely found, having been reported in only one case[11].
Clinical diagnosis
Diagnosis of FEP is not difficult, but misdiagnosis can occur because of a doctor's incomplete examination. If a laboratory examination reveals an upper urinary tract obstruction without the presence of a calculus, FEP should be primarily taken into considerasion. Most cases have complications of hydronephrosis. Banner and Pollack [12] considered radiology to be a suitable procedure, while Kim et al[13]. preferred flexible ureter cystoscopy to be the best means. Typically, X-rays of FEP show a long thin filling defect. In our case, intravenous urography (IVU) revealed a filling defect in the ureter with a smooth and sharply demarcated outline. Of course, histological diagnosis confirmed the result. In general case, most FEP are long slender projections grossly with a smooth surface presenting as single or multiple villiform segment with a maximal length of 13 cm. In our case, a polyp of 7 cm long appeard. Some have claimed they can be long enough to enter into the bladder[14]. Microscopically, FEP arise from the submusoca and are composed of a loose connective tissue core covered by a layer of normal urothelium. The central edematous stromal stalk contains collagen smooth muscle fibers, fibroblasts and acute and chronic inflammatory cells meet occasionally, even some irregular star-like polynucleated cells, which may cause misdiagnosis. The polyps are connected with the ureteral wall. They have a wider stalk and looser connective tissue compared to a papillary urothelial neoplasm, and a few acute and chronic inflammatory cells may be found.
Differential diagnosis
Tn flammatory polyps
The main difference between FEP and inflammatory polyps lies in infection in the peripheral tissue. Microscopically, just like tiny angioma, inflammatory polyps have a rich blood supply with plentiful acute and chronic inflammatory cells. The urothelium occasionally exhibits hyperplasia or metaplasia.
Papillary urothelial neoplasm
It is a polyloid mass with a low malignancy potential that originates from the urothelium with a long stalk. Microscopically, these lesions are made up of a core of fibrovascular stroma emerging from the submusoca and covered by normal transitional epithelium. The stalk is thinner and the fibroconnective tissue is looser than that of FEP. Observed from a longitudinal section, every villus is covered by more than 5 layers of transitional epithelium, but it is free of atypia.
Inverted transitional cellular papilloma
This is a benign urothelial tumor that has an inverted growth pattern with normal or minimal cytologic atypia of the neoplastic cells. Inverted transitional cellular papilloma looks like a benign tumor with a long stalk which is covered by normal urothelium. The tumor cells are free of atypia.
Transitional cellular carcinoma
Differentiating FEP from transitional cellular carcinomas is very important because of their opposite nature which has a life-and-death impact on a patient's life span. In general, the urothelium contains abnormal cells, exceeding the thickness of normal urothelium in transitional cellular carcinoma. In some cases, invagination and infolding of normal urothelium trapped within the stroma can be seen.
Treatment and prognosis
FEP are nonepithelial tumors that originate from mesodermal tissue of the ureteral wall. No reported cases of recurrence after local resection have been found in the literature. Many surgical approaches have been advanced for benign polyps. Low grade FEP can shrink by removing the obstruction and control of the infection. Because of their benign nature, surgical therapy should be limited and conservative if the kidney function is normal; otherwise, nephroureterectomy should be performed. On follow-up examinations at nine years after surgery, tumor recurrence and canceration were not detected[15]. Recently, with the development of molecular pathology, a new suggestion has been posted: a follow-up examination has been recommended if P53 and (or) c-myc were positive immunohistochemically. These findings may indicate a malignancy potential[15].
- Received August 1, 2006.
- Accepted September 27, 2006.
- Copyright © 2006 by Tianjin Medical University Cancer Institute & Hospital and Springer