Abstract
OBJECTIVE To clarify the expression of MTDH in invasive micropapillary carcinoma of the breast (IMPC) and analyze the relationship between MTDH expression and clinicalpathologic parameters of the IMPC patietns.
METHODS The expression of MTDH protein was analyzed using immunohistochemical staining in 86 cases with IMPC and another 86 cases with invasive ductal carcinoma not otherwise specified (IDC-NOS). The association between MTDH expression and clinicalpathologic parameters of the IMPC patients was analyzed.
RESULTS Immunohistochemical analysis revealed the high expression of MTDH in 64 of the 86 (64/86, 74.4%) IMPC patients and in 45 of the 86 (45/86, 52.3%) IDC-NOS patients. Statistical analysis showed a statistically significant difference in MTDH expression between IMPC and IDC-NOS (P < 0.05). In IMPC, the expression of MTDH was correlated with lymph nodes metastasis (P < 0.05). The expression of MTDH was negative in normal breast tissue of IMPC and IDC-NOS patients.
CONCLUSION High expression of MTDH is one of the molecular mechanisms, which facilitates lymph node metastasis of IMPC, therefore, the expression level of IMPC plays an important role in lymph node metastasis of IMPC.
keywords
Introduction
Metadherin (MTDH), also known as astrocyte elevated gene-1 (AEG-1), is a new oncogene found in recent years. Published studies have suggested that MTDH expression is up-regulated in several kinds of tumors, such as breast cancer, prostate cancer, non-small cell lung cancer, squamous cell carcinoma and renal cell carcinoma et al.[1–5] and the level of the MTDH expression is associated with tumor invasion and metastasis. Importantly, MTDH enhances the invasiveness of breast cancer cells by inducing epithelial to mesenchymal transition[6].
Invasive micropapillary carcinoma (IMPC) is a rare and histological special type of breast cancer with high prevalence of lymphovascular invasion, high incidence of lymph node metastases and poor prognosis[7–10]. In the resent study, Li et al.[11] found that the increased proportion of CD44+/CD24–/low tumor cells and the epithelial-mesenchymal transition may play an important role in tumor invasion and metastasis of breast IMPC.
To our knowledge, evaluation of the expression of MTDH in breast IMPC has never been reported before. For this reason, in this study, the expression of MTDH protein was examined in 86 cases diagnosed as IMPC and in a control group of another 86 cases diagnosed as invasive ductal carcinoma not otherwise specified type (IDC-NOS) using immunohistochemistry, and the association between MTDH expression and lymph node metastasis of IMPC was discussed in this paper. Furthermore, we attempted to further investigate the potential role of MTDH in lymph node metastasis of breast IMPC.
Materials and Methods
Specimens
The paraffin-embedded tumor samples taken from 86 cases with breast IMPC (pure IMPC 23 cases, concurrent IMPC and IDC-NOS 63 cases) and from another 86 cases with IDC-NOS were obtained from the Department of Breast Cancer Pathology and Research Laboratory, Tianjin Medical University Cancer Hospital (Tianjin, China). The patients in both groups were diagnosed during 2008. All the patients were women and their age ranged from 23 to 80 years, with a mean age of 52. None of them had received preoperative radiotherapy or chemotherapy. All the specimens were fixed in 10% formaldehyde and embedded in paraffin. The histopathology was reviewed and then the diagnosis of each case was made and confirmed independently by 3 pathologists[12] based on the 2003 World Health Organization histologic classification of tumors of the breast[13]. The IMPC specimens were divided into 4 groups according to the amount of IMPC presenting in each tumor: IMPC accounting for less than 25% of the whole tumor, for 25%–49%, for 50%–75%, and for more than 75%[11].
Reagents
Rabbit anti-MTDH, mouse anti-ER and PR, kit for immunohistochemical indirect method and DAB substrate kit were all purchased from Beijing Zhongshan Golden Bridge Biotechnology Co. Mouse anti-HER2 (1:800) was purchased from Newmarkers.
Staining methods
Immunohistochemical (IHC) staining was performed using the labeled streptavidin-biotin method (LSAB). The MTDH primary antibody was diluted at 1:500, and the ER, PR, HER2 primary antibody was diluted at 1:150, 1:150 and 1:800, respectively. All antigens were restored with high-pressure cooking in citrate buffer (pH 6.0) for 2.5 min before they were blocked with the serum. The 3.3′-diaminobenzidine (DAB) was used to show the reaction intensity, and hematoxylin was used for counterstain of the sections. Phosphatebuffered saline (PBS) was used instead of primary antibody in the incubation step as a negative control, and the positive controls were used according to the manufacture’s recommendation.
Standardization assessments of the results
The degree of immunostaining of formalin-fixed, paraffin-embedded sections was reviewed and scored independently by 2 observers, based on both the proportion of positively stained tumor cells and the intensity of the stain[14,15]. MTDH[2] immunohistochemistry labelled the cytoplasm of tumor cells, the proportion of tumor cells was scored as follows: 0 (no positive tumor cells), 1 (positive tumor cells < 10%), 2 (positive tumor cells between 10%–50%), and 3 (positive tumor cells > 50%). The stain intensity was graded according to the following criteria: 0 (no stain), 1 (weak stain − light yellow), 2 (moderate stain − yellow brown), and 3 (strong stain − brown). The staining of MTDH was calculated as staining intensity score × proportion of positive tumor cells, and the scores were in the range of 0, 1, 2, 3, 4, 6, and 9. The staining index score of ≥ 4 demonstrated that there was a high expression of MTDH in the tumor and that of ≤ 3 indicated a low expression of MTDH in the tumor, and that of 0 showed none or negative. Cases were scored positive for ER and PR if nuclear immunoreactivity was present in > 10% of tumor cells[16]. The scoring of HER2 was as follows[17]: Strong, circumferential membrane staining demonstrated in more than 30% of the invasive carcinoma cells was scored as 3+; moderate, circumferential membrane staining demonstrated in 10% or more of the invasive tumor cells or 3+ staining in 30% or less of the invasive tumor cells was scored as 2+ staining; weak and incomplete membrane staining presented in the invasive tumor cells was scored as 1+; and no staining shown in the tumor invasive cells was scored as 0. In the IMPC group, only the staining of the IMPC component was evaluated.
Statistical analysis
Data were analyzed using SPSS 15.0 software package. The methods of statistical analysis were mainly Mann-Whitney U-test, χ2 test and Spearman’s rank correlation test. P < 0.05 was considered statistically significant in all the statistical analyses.
Results
Clinical information
Among the 86 cases with IMPC (pure IMPC 23 cases, concurrent IMPC and IDC-NOS 63 cases), there were 32 cases with the IMPC component accounting for less than 25% of the primary tumor, 8 cases with the IMPC component for 25%–49%, 18 cases for 50%–75% and 28 cases for more than 75%.
Compared with the IDC-NOS patients in the control group, IMPC patients had larger tumor size (Z=−4.351, P−0.000, Table 1) and a higher rate of lymph node metastasis (Z=−5.893, P=0.000, Table 1). Among IMPC patients, 73 (73/86, 84.9%) cases exhibited lymph node metastasis. However, only 36 IDC-NOS patients (36/86, 41.9%) had nodal metastasis. Noticeably, of the 73 cases with breast IMPC exhibiting nodal metastasis, 46 cases with their metastatic carcinoma presenting in the lymph nodes was diagnosed as IMPC, 21 cases diagnosed as concurrent IMPC and IDC-NOS and 6 cases diagnosed as IDC-NOS. The rate of lymph node metastasis of the amount of IMPC component in primary tumour varied from < 25%, 25%–49%, 50%–75% and > 75% was 93.8% (30/32), 87.5% (7/8), 72.2% (13/18), 82.1% (23/28), respectively. No correlation was found between the amount of IMPC components in the primary tumor and the rate of lymph node metastasis of the primary tumor (rs =−0.157, P = 0.149).
The various pathologic parameters between IMPC and IDC-NOS.
Expression of MTDH in IMPC and IDC-NOS
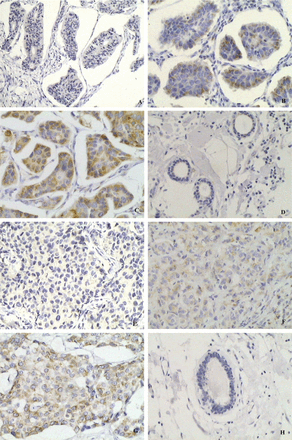
In the 86 cases with IMPC, high expression of MTDH was demonstrated in 64 cases (64/86, 74.4%), low and none expression of MTDH presented in 22 cases (22/86, 25.6%), and the negative expression of MTDH shown in normal breast tissue of the IMPC patients (Fig.1A–D). No significant association was observed between the amount of IMPC components in the primary tumor and the expression level of MTDH (rs =−0.078, P = 0.476). In contrast, in the control group, only 45 IDC-NOS cases (45/86, 52.3%) presented high expression of MTDH, 41 cases (41/86, 47.7%) showed low or none expression of MTDH. MTDH expression was negative in the normal breast tissue of the IDC-NOS patients (Fig.1E–H). Compared with IDC-NOS, IMPC showed significantly higher expression of MTDH (χ2 − 9.042, P = 0.003, Table 2). Of the 86 cases with IMPC, the rate of lymph node metastasis in the patients exhibiting high expression of MTDH was 90.6% (58/64), and that in the patients exhibiting low or none expression of MTDH was 68.2% (15/22). MTDH expression was positively correlated with lymph node metastasis in the IMPC patients (P = 0.011). No correlation was found between the expression of MTDH and each of tumor size, ER, PR and HER2 (P > 0.05, Table 3).
A, Negative expression of the MTDH protein in IMPC (IHC LSAB, ×200); B, Low expression of the MTDH protein in IMPC (IHC LSAB, ×200); C, High expression of the MTDH protein in IMPC (IHC LSAB, ×200); D, Negative expression of the MTDH protein in normal breast tissue of IMPC (IHC LSAB, ×200); E, Negative expression of the MTDH protein in IDC-NOS (IHC LSAB, ×200); F, Low expression of the MTDH protein in IDC-NOS (IHC LSAB, ×200); G, High expression of the MTDH protein in IDC-NOS (IHC LSAB, ×200); H, Negative expression of the MTDH protein in normal breast tissue of IDC-NOS (IHC LSAB, ×200).
Expression of MTDH in IMPC and IDC-NOS.
The relationship between the expression of MTDH and the various pathologic parameters in IMPC.
Discussion
MTDH, a Ha-ras regulated gene, located at chromosome 8q22, was originally identified by Su et al. as a protein induced in primary human fetal astrocytes infected with HIV-1 or treated with HIV gp120 or tumor necrosis factor-α[18–20]. It contained 12 exons and 11 introns with a full-length of 86,082 bp and pI 9.3[21]. Additional studies have shown that MTDH could promote tumor progression, including transformation, initiation of apoptosis, invasion, metastasis, chemoresistance and angiogenesis through many signaling pathways, such as the phosphatidylinositol-3-kinase/Akt pathway, the Rac/Rho pathway, the Rac/c-Jun-NH2-kinase, and Rac/p38 pathways, et al.[22,23] Our present study demonstrated that the expression level of MTDH was related to lymph node metastasis of IMPC, suggesting that MTDH might promote the invasion and metastasis of tumor cells in IMPC by some signaling pathways.
It has been found that the expression level of MTDH is elevated in many types of human malignancy, including breast cancer, prostate cancer, non-small cell lung cancer, squamous cell carcinoma and renal cell carcinoma et al.[1–5], and its high expression is related to tumor invasion and metastasis. Importantly, some reports on breast cancer have demonstrated that MTDH enhances the invasiveness of breast cancer cells by inducing epithelial to mesenchymal transition (EMT)[6]. Some studies have suggested that EMT could generate breast cancer stem cells[24,25]. Breast cancer cells with a CD44+/CD24−/low phenotype has been associated with stem cell-like characteristics, such as enhanced invasive properties[26,27]. Recently, our study has revealed that CD44+/CD24−/low tumor cells in IMPC may arise through an EMT transdifferentiation process[11]. In addition, the growing pattern of the micropapillary group might be the initial stage of the EMT[28]. It seems reasonable, therefore, to hypothesize that MTDH could promote the invasion and lymph node metastasis of IMPC through EMT. In addition, the previous studies have demonstrated that there were many microvessel in IMPC[29] and the VEGF-C high expression was associated with lymph node metastasis of IMPC[30]. The significance of MTDH expression was in correlation with VEGF in triple-negative breast cancer[31]. MTDH is indeed a direct regulator of angiogenesis by up-regulating key components, such as vascular endothelial growth factor (VEGF), which plays an important role in the process of blood vessel formation[32,33]. Therefore, we assume that MTDH could promote lymph node metastasis of IMPC by upregulating VEGF. These notions are supported by the findings from this present study, in which MTDH expression was shown much higher in IMPC than in IDC-NOS and the expression level of MTDH was associated with lymph node metastasis of IMPC.
The expressions of MTDH in normal breast tissue, UDH (usual ductal hyperplasia), ADH (atypical ductal hyperplasia), DCIS (ductal carcinoma in situ) and invasive breast cancer are significantly different, suggesting that the overexpression of MTDH may contribute to breast cancer progression[34]. MTDH expression is higher in breast tumors than in normal breast tissue at mRNA and protein level and there is significant association between MTDH expression and each of tumor size, clinical stage and lymph node metastasis[2]. In addition, MTDH expression is higher in renal cell carcinoma than in the paired normal tissue from the same patient and is correlated with tumor grade, clinical stage and TNM classification[5]. Song et al.[35] also found that MTDH expression was markedly correlated with TNM classification and histological differentiation in colorectal carcinoma. The results in our present study also reveals that the expression of MTDH is closely correlated with lymph node metastasis of IMPC. No correlation was found between the expression of MTDH and each of tumor size, ER, PR and HER2 in IMPC. These studies have provided new insights into the potential role of MTDH in the invasion and metastasis of IMPC, and high expression of MTDH is one of the molecular mechanisms, which facilitates lymph node metastasis of IMPC.
It is remarkable that a new report reveals that MTDH DNA vaccine could effectively inhibit the growth and metastasis of breast cancer[36]. This indicates that it has provided new strategies for clinical treatment of breast cancer.
The expression of MTDH is negative in normal breast tissue, and high in breast cancer cells, so it might be a potential diagnostic marker and therapy target in breast cancer. Further studies are needed to investigate large size of the sample that comprises other histological types of breast cancer in order to validate the findings obtained in this present study and to further explore the place of MTDH for the purpose of predicting prognosis and monitoring response to the therapy of the breast cancer patients.
Conflict of interest statement
No potential conflicts of interest were disclosed.
Acknowledgments
This work was supported by National Natural Science Foundation of China (No. 30930038), Program for Changjiang Scholars and Innovative Research Team in University (No. IRT0743), National High Technology Research and Development Program (“863”Program) of China (No.2006AA02A249), National “973” program of China (No. 2009CB521700).
- Received April 21, 2011.
- Accepted May 19, 2011.
- Copyright © 2011 by Tianjin Medical University Cancer Institute & Hospital and Springer