keywords
Introduction
China is a country with a low morbidity of prostate carcinoma. The incidence of prostate carcinoma in China is 1.6/100,000, which is much lower than the rate in the United States, i.e., 119.9/100,000 [1]. Due to changes of lifestyle and improved measurement of serum prostate specific antigen (PSA) over the past decades, the incidence of prostate carcinoma in China also showed a yearly increase. However, the misdiagnosis and mistreatment of this disease commonly occur. The aim of this study is to report the case of a patient with prostate carcinoma presenting asymptomatic but with left supraclavicular lymphadenopathy, and analyze the reasons of misdiagnosis and mistreatment.
Case Report
A 65-year-old male, previously fit and well, was admitted to an oncological out-patient clinic with persistent left supraclavicular lymphadenopathy. He complained that had a 1-week history of an asymptomatic left neck masses. Physical examination revealed lymph node swelling in the left supraclavicular fossae without lymph nodes in the axillae or groins. Examination on his chest and abdomen were normal. A digital rectal examination (DRE) was not performed at the time. The diagnosis of a malignant lymphoma or Troisier sign was strongly recommended and he was admitted to a hematology medical ward.
Without definite evidence for diagnosis, a biopsy of cervical lymph nodes was performed. The specimen showed a lymph node extensively replaced by metastatic adenocarcinoma cells. His chest X-ray and electronic daryngopharyngeal mirror examination were normal. The digestive tract radiography showed a soft tissue in goiter outside the rectum. An ultrasound scan on his neck and abdomen found multiple, large lymph nodes in the left neck and supraclavicular fossa, the largest node measuring 2.5 cm, with multiple lymphadenopathy in the retroperitoneal space. Three months later, a computed tomographic (CT) scan disclosed multiple lymph nodes enlarged in the retroperitoneal space and that areas of hibateral iliac blood vessels regions. Five months later, a CT scan showed enlarged fused lymph nodes in right iliac blood vessels region with thickness of the bladder posterior wall. Repeated blood analyses and bone marrow biopsies were normal.
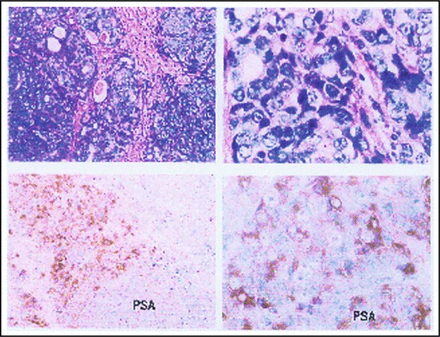
One year later, immunohistochemistry staining for prostate-specific antigen (PSA), AFP, CK20, CK7, Tg, CEA were performed in enlarged left supraclavicular lymph nodes from the biopsy tissues. This showed the lymph nodes extensively replaced by metastatic adenocarcinoma cells that were stained positive for prostatespecific antigen PSA (Fig.1), and shown negative for AFP, CK20, CK7, Tg, CEA. He then had a digital rectal examination which confirmed a hard, abnormal prostate. The level of serum total prostate-specific antigen (PSA) had risen to over 100 ng/ml, free PSA over 30 ng/ml, and a bone scan suggested a metastatic disease. MRI examination of the prostate suggested that a lesion of low signal intensity on T2-weighted images that contrast with the high-signal intensity peripheral gland, and abnormalities of the prostatic capsule. The T2-weighted image also showed abnormally low signal intensity involving the left seminal vesicle. To confirm the diagnosis, six core needle prostate biopsies were performed which revealed a Gleason score of 8/10 adenocarcinoma of the prostate. Thus the diagnosis of prostate carcinoma was confirmed.
Immunohistochemical staining showed positive for PSA in lymph node tissues.
Previously, the patient had been mistreated with CHOP (cyclophosphamide, hydroxydaunorubicin, and prednisone) regimen for malignant lymphoma for some time, but treatment results were not satisfactory. Since the diagnosis of prostate carcinoma was proven, the patient was started on Flutamide 250 mg, three times a day and Goserelin Acetate Implant injections 3.75 mg, monthly. Three months later, the patient had significant symptomatic relief with a remarkable reduction in supraclavicular lymphadenopathy and a decreased total prostate-specific antigen level of 1.6 ng/ml, free PSA 0.46 ng/ml.
Discussion
Prostate carcinoma is known to blood stream via three ways: local invasion, hematogenous dissemination, and lymphatic metastasis. Local invasion of prostate carcinoma into the urethra, bladder neck, and trigone and seminal vesicles is common. The rich venous plexus of Batson is implicated as the route of hematogenous dissemination of prostate adenocarcinoma to the pelvic bones, femur, lumbar spine, thoracic spine and ribs. Lymphatic spread to the obturator, hypogastric, iliac, presacral and para-aortic nodes is a common route of metastasis[2]. Metastasis through supraclavicular lymph node is uncommon in patients with prostate carcinoma[2,3]. Rare case reports described cervical lymph node metastasis to the first clinical manifestation of prostate carcinoma, but only appear in the cases with a widely dissemination[4]. Metastasis to supraclavicular lymph nodes (SLN) mainly occurs in lung carcinoma, digestive tract tumor, breast carcinoma etc, but rarely in prostate carcinoma[5]. This patient had been misdiagnosed and mistreated as primary malignant lymphoma. Saeter et al.[6] reported that, in 35 patients with non-regional lymphatic spread from prostate carcinoma, 69% of them had metastasis to the supraclavicular fossa.
Serum prostate specific antigen (PSA) measurement and immunohistochemical PSA staining have been proven to be a reliable means of establishing the diagnosis of metastatic prostate carcinoma[7]. As prostate carcinoma screening index, PSA-based screening for prostate carcinoma has obvious advantages that others cannot substitute. Due to its significant applicability for early detection, risk prediction, and follow-up evaluation, PSA has revolutionized our ability to treat prostate carcinoma patients[8,9]. Though immunohistochemical staining with PSA can react with the vast majority of primary and metastatic prostate carcinomas, poorly differentiated prostatic carcinomas tend to stain less extensively than do more well-differentiated carcinomas[10,11]. Confirmed prostate carcinoma diagnosis is established by biopsy tissue immunohistochemical PSA specific staining, serum PSA measurement, needle biopsies, and MRI examination of the prostate.
In this case report, there was a delay of diagnosis for one year before it was confirmed. The patient experienced repeated complete blood count, bone marrow biopsies, basic chemistry, and ultrasound and computed tomographic (CT) scans. However, he did not have a digital rectal examination or a serum prostate-specific antigen level check until the result of PSA staining indicated that the primary site was the prostate.
Conclusion
Prostate carcinoma with metastasis should not be overlooked when metastatic adenocarcinoma is discovered in the supraclavicular lymph nodes of old men. Although metastatic prostate carcinoma of the supraclavicular lymph nodes is rare, it should not be ruled out, because it may be hormonally responsive. We recommend that a digital rectal examination and serum prostate-specific antigen measurement be performed at the time of initial presentation. Prostate carcinoma may be ruled out using immunoperoxidase stain for PSA. The confirmed diagnosis can be established by prostate biopsy and a MRI of prostate.
- Received September 24, 2008.
- Accepted November 12, 2008.
- Copyright © 2008 by Tianjin Medical University Cancer Institute & Hospital and Springer