keywords
Introduction
Nodular lymphocyte predominant Hodgkin’s disease occurs in 5% of all cases of Hodgkin’s disease. It occurs more commonly in male. Only 5% of all Hodgkin’s lymphoma cases develop spinal cord compression[1] and in only 0.2% cases, spinal cord compression occurs as the initial presentation[2]. So our case is rare both in the form of the unique variety of Hodgkin’s disease and also in the form of presentation.
Case report
A 45-year-old female presented with 1-month history of dull aching pain in low back, which was gradually increasing, radiating to left lower limb and was radicular in nature. She also felt unsteady gait and gradually progressive both lower limbs weakness without any bladder or bowel involvement. There was neither any history of fever or weight loss nor any past history of tuberculosis. She was neither diabetic nor hypertensive.
Clinical examination revealed a lymph node of 3 cm in diameter in left axillary region, which was not tender, rubbery in consistency, not fixed to the skin or underlying structures, and firm hepatomegaly with sharp margin and irregular surface, 3 cm below right costal margin in mid-clavicular line and firm splenomegaly 4 cm below left subcostal margin along the splenic axis were detected. She also had mild pallor and kyphosis of the spine with tenderness over lumbar vertebrae 3-4. Patient’s mental status was absolutely normal. Other neurological examinations revealed-no cranial nerve palsy, or flexor plantar response, weakness of the muscles innervated by the compressed roots, power of grade 3/5 in both lower limbs with normal power in upper limbs, decreased tone with absent deep tendon reflexes in lower limbs, saddle anesthesia, bilateral leg pain and weakness.
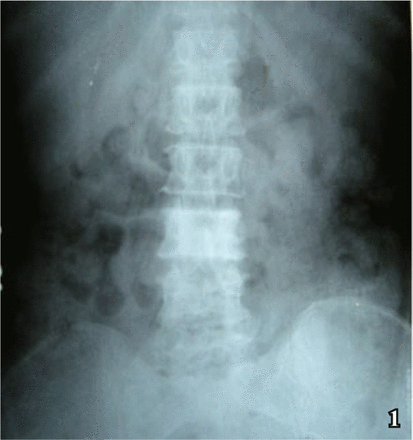
Laboratory investigations revealed-normal levels in hemogram, blood sugar level, urea, creatinine, sodium and potassium. Liver function test was normal except raised alkaline phosphatase (359 U/L). Other blood biochemistry tests were as follows: LDH 691 U/L (N-< 378), uric acid 7.3 mg/dL (N-2.6-6.0), calcium 8.39 mg/dL (N-8.0-10.5) and phosphate 4.20 mg/dL (N-3.O-5.0). Chest x-ray was normal. Ultrasonography of whole abdomen showed - hepatomegaly with an ill-defined hypoechoic area in right lobe adjoining gall bladder and enlarged spleen with multiple hypoechoic lesions of varying sizes. No intraabdominal lymphadenopathy was detected. X-ray of lumbar spine showed sclerotic lesion in the 3rd lumbar vertebra (Ivory vertebra) (Fig. 1). CT scan of whole abdomen confirmed the ultrasonographic findings of hepatosplenomegaly with low density areas in the liver (Fig. 2) and the spleen, raising the probability of lymphoproliferative disorder and also a sclerotic lesion in the 3rd lumbar vertebra likely indicating a neoplasm. MRI of lumbosacral spine was performed to detect the exact pathology, which revealed-infiltration of marrow of lumbar vertebrae 3, 4 and 5, a soft tissue mass in posterior aspect of the 3rd lumbar vertebra causing extradural compression on the thecal sac at this level and posterior disc bulge at lumbar 3-4, lumbar 4-5 and lumbar 5, that was the sacral 1 level. No mediastinal lymphadenopathy, hilar enlargement, or pulmonary parenchymal lesions were detected. CT scan of the brain was normal. The tests for human immunodeficiency virus antibody and carcinoembryonic antigen were negative; venereal disease research laboratory test was nonreactive in this patient. CT guided FNAC from hepatic space occupying lesion (SOL) and the 3rd lumbar vertebra (Fig. 3) were performed, which did not guide us to reach to the exact tissue for diagnosis.
X-ray of lumbosacral spine (AP view) showing sclerotic 3rd lumbar vertebra (Ivory Vertebra).
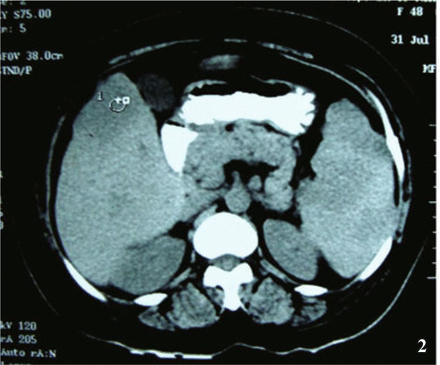
CECT scan of upper abdomen showing hepatosplenomegaly with low density areas in the liver.
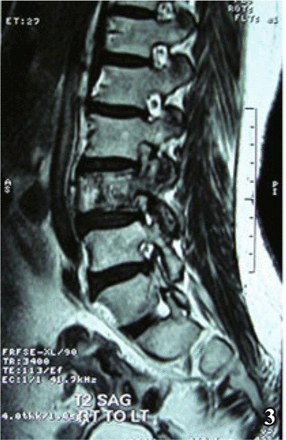
CT scan of the lumbosacral spine showing distorted normal architecture of 3rd lumbar vertebra.
Then we planned to perform left axillary lymphnode biopsy. The histopatholgic examination revealed a mass that was composed of multiple oval to round cells separated by bands of sclerotic collagen along with focal sclerosis. The node was composed of numerous neutrophils, plasma cells, histiocytes, and small, relatively benign-appearing lymphocytes. In addition, there were varying numbers of large atypical mononuclear cells. Many of these cells had vesicular nuclei with single prominent nucleolus. At this stage, we diagnosed the patient to be suffering from Hodgkin’s Disease (HD), Stage IV and eagerly waited for the immunohistochemistry results. Immunohistochemistry confirmed the diagnosis of “Nodular, lymphocyte predominant type of Hodgkin’s lymphoma”. The Lymphocytic and Histiocytic cells (L&H cells) expressed CD20, OCT2 & EMA and immunonegative for CD30, CD15 & MUM-1. To know the extent of the disease, a bone marrow biopsy was performed, which revealed bone marrow infiltration by lymphoproliferative disorder with mild focal myelofibrosis.
The patient was treated successfully with ABVD (Adriamycin, Bleomycin, Vinblastine, Dacarbazine) regimen of chemotherapy with a clinical complete response. Chemotherapy was well tolerated and she was relieved from symptoms and signs of nerve compression just after the completion of single cycle of chemotherapy. She received 8 cycles of the same regimen. MRI of the lumbosacral spine was obtained shortly after the completion of the third cycle of chemotherapy, which revealed a complete resolution of the mass lesion. However, lumbar vertebral sclerotic changes did not subside. Subsequent MRI scans after all cycles chemotherapy did not detect further changes. After completion of chemotherapy, external beam radiation therapy was delivered to the lumbar spine with a single posterior field surrounding the 3rd lumbar vertebral body. Twenty fractions were delivered over 1 month.
When the patient was last seen in follow-up, 12 months after completion of external beam radiation therapy, her only complaint was that she had a mild feeling of heaviness in left upper abdomen. The patient now is completely ambulatory and her clinical examination is within normal limits except for persistence of hepatosplenomegaly.
Discussion
Nodular lymphocyte predominant Hodgkin’s lymphoma (NLPHL) is a form of lymphoma[3]. Nowadays, it is not classified as a variant of classic hodgkin’s disease (HD). This is because the fact that Reed-Sternberg Cell (RSC) variants (popcorn cells) that is characteristics of this form of disease always express B lymphocyte marker, such as CD20, thus making NLPHL an uncommon form of B cell lymphoma. However, the most fatal consequences that might complicate this form of disease (unlike classic HL) is progression to diffuse large B cell lymphoma. Small but clear differences in prognosis between the various forms are noted. Lymphocyte predominant HL is a very uncommon subtype of HL, which was composed of nodules containing numerous small reactive lymphocytes mixed with large popcorn-shaped RSC. Unlike classic RSC, the non-classic RS cells of NLPHL are CD15 and CD30 negative, though they are highly positive for the B cell marker CD20. Despite the difficulty in identifying Reed-Sternberg cells on histologic examination and the absence of immunohistochemical stains for T-cell markers in our case study, the complete histologic findings was most consistent with a diagnosis of nodular, lymphocyte predominant type of Hodgkin’s lymphoma, a very rare form of the disease.
Central nervous system involvement by HD is a very uncommon manifestations, and central nervous system clinical features of HD are extremely rare[4]. Spinal cord along with radicular compression is a rare complication of HD, affecting nearly 5% of all cases[1]. Spinal cord involvement usually demonstrates the progression of advanced disease similar to that of intracranial spread. Our case history represents a relatively unique case of HD (Nodular, lymphocyte predominant type of Hodgkin’s lymphoma) presenting with extradural disease and lumbar radicular compression as the only site of initial clinical involvement. Undoubtedly, this is an extremely rare presentation (0.2%)[4]. Few cases reported in the literature are available, which describe spinal cord or radicular compression as the initial clinical manifestation of HD[4].
Contiguous spread from paravertebral masses through the vertebral foramen is the pathway of entrance of lymphoma into the epidural space[4]. The presence of an area of increased attenuation in the paravertebral lumbosacral region on MRI scan in this case study confirms that this is the mechanism of spread of lymphoma cells to the epidural space causing features of radiculopathy. These paravertebral lesions might be mediastinal or retroperitoneal group of lymph nodes. Secondary to lymphomas, the vertebral bodies are often remain unaffected, therefore, plain films might be normal, in epidural spinal cord compressive myelopathy[4]. However, in our case study, we noticed single sclerotic vertebral body in plain film, which was commonly known as ivory vertebra that persisted even after the course of therapy was completed.
In the spinal cord, thoracic segment is most commonly affected, followed by lumbar and rarely the cervical region[5]. Since, in the neck, lymphoma would manifest as a visible mass before causing compressive myelopathy. Apart from features of compressive myelopathy, neurologic features of ‘transverse myelitis’ may occur rarely due to interruption of blood supply of the intervertebral foramen. It is reported that bone marrow involvement in Hodgkin’s lymphoma occurs in 5%-15% of cases[6]. This unusually high incidence of marrow involvement predicts widespread and advanced stage of disease at the time of presentation.
To come to a diagnosis of Hodgkin’s lymphoma, one should find the characteristic group of cells-lymphocytes, plasma cells, histiocytes and eosinophils; as well as mononuclear and binucleate Reed-Sternberg cells. The differential diagnosis of Hodgkin’s lymphoma presenting as radiculopathy would include tuberculosis, Non-Hodgkin’s lymphoma (NHL), non-specific inflammation, and rarely eosinophilic granuloma[7].
Clinically observed response of neurologic symptoms along with resolution of disease after 8 cycles of chemotherapy supported the diagnosis of HD. In this case study, we saw that the patient complained a severalmonth gradually progressive lower limb weakness, low back pain, and gait disturbance before the definitive diagnosis of cauda equina syndrome. In contrast to cases developing carcinomatous invasion of the extradural space, duration of onset of symptoms before the development of spinal nerve root compression caused by lymphoma cells might be surprisingly long, often extending from months to years[1].
The definitive management of cauda equina syndrome induced by HD needs a thorough and multidisciplinary approach. Standard management protocol includes local radiation therapy with or without surgical intervention. Nowadays, chemotherapy has become the mainstay of treatment or in combination with local radiation therapy. It is quite evident that radiotherapy is an integral part in the management of most HD patients presenting with spinal nerve root compression. A variety of time-dose radiation therapy have been used regularly to treat HD presenting with spinal nerve compressive symptoms[8]. Chemotherapy alone represents another clinical option for HD presenting with spinal cord compression. Burch and Grossman[9] reported 2 cases of epidural spinal cord compression, occurring in the background of relapsed HD and noticed dramatical response to systemic chemotherapy alone. Since HD rarely presents with spinal cord compression (0.2% initial presentation and 5% overall), none of the available data clearly defines the optimal treatment for HD presenting with spinal cord compression. In general, however, the effectiveness of combined-modality therapy for advanced HD remains controversial[10]. Role of surgical intervention must be individualized. In our case study, we first tried for CT-guided FNAC from paravertebral lesion to obtain sufficient material to establish a pathologic diagnosis. However, elective surgery was not performed. Although HD patients presenting with initial spinal cord compression are very rare, this clinical setting represents one situation that surgery might be inevitable.
Survival benefit of this patient is also very important. Perry et al.[4] described 2 patients with HD who presented with spinal cord compression as the first clinical manifestation of disease. Survival of each of them was 32 and 79 months, respectively. In the study led by Silverberg and Jacobs[11] among 5 HD patients with spinal cord compression, the absolute 3-year survival rate was 60%. One of these patients’ survival was over 6.5 years. It is quite evident, that long term survival is not uncommon in HD patients presenting with cauda equina syndrome.
In our present case study, the lumbar spine was the involved site, though it is not the commonest one. Tissue diagnosis of Hodgkin’s lymphoma manifesting as compressed radiculopathy requires awareness of the condition, since proper evaluation and early initiation of therapy may alter the life expectancy of these patients. Detailed clinical evaluation including history of previous biopsy, status of lymph nodes, liver, spleen are essential for the staging of the disease. The diagnosis becomes easy, when past history of Hodgkin’s lymphoma is available. Since, nodular, lymphocyte predominant type of Hodgkin’s lymphoma may progress to diffuse large B cell lymphoma, we should remain vigilant regarding this fact during evaluation of patients. However, when cord compression is the first clinical feature, the diagnosis becomes tough and the tissue should be carefully examined. There are few case studies showing spinal cord compression in classical Hodgkin’s disease, however, there are no such documentation in nodular, lymphocyte predominant type of Hodgkin’s lymphoma, which is a very rare variety. Our case study is the first one to document this neurologic complications in this rare form of disease. Therefore, our case study is a rare one and the first one, both in the form of the unique variety of Hodgkin’s disease and also in the form of presentation.
Conflict of interest statement
No potential conflicts of interest were disclosed.
- Received October 10, 2010.
- Accepted October 18, 2010.
- Copyright © 2010 by Tianjin Medical University Cancer Institute & Hospital and Springer