Abstract
OBJECTIVE To study the clinical, pathologic and imaging features of multilocular cystic renal cell carcinoma (MCRCC) and to review the diagnosis and treatment of this subtype of renal cell carcinoma (RCC).
METHODS The data from 8 cases (mean age, 49.4; 5 men and 3 women) who had been treated from 2004 to 2006, were reviewed retrospectively. Radiologic and pathologic documents were evaluated. For treatments, radical nephrectomy was conducted in 4 patients, partial nephrectomy in 2 and laparoscopic nephrectomy in 2.
RESULTS Postoperative pathological findings confirmed the diagnosis of MCRCC. The stage of all 8 cases was pT 1. For pathologic grade, 7 cases were G1 and 1 case was G2. Seven patients available for follow-up had survived tumor-free during the mean time of 8 months.
CONCLUSION MCRCC is an uncommon subtype of RCC, it has a lower malignant potential and a better prognosis compared with other types of RCC. Nephron-sparing surgery may be an appropriate treatment options for MCRCC.
keywords
Multilocular cystic renal cell carcinoma( MCRCC) is a relatively rare cystic tumor of the kidney. Because of its distinct characteristics in prognosis and natural history, MCRCC was recognized as a seperate subtype of renal cell carcinoma in the 2004 WHO classification of adult kidney tumors [1]. The aims of this study were to assess the presentation, diagnosis and treatment options for MCRCC based on our review of 8 cases.
MATERIALS AND METHODS
For this retrospective study, the samples were obtained through the Second Hospital of Tianjin Medical University from 2004 to 2006. Eight cases diagnosed as MCRCC according to the 2004 WHO criteria were included.
Clinical and demographic information obtained through the hospital records included clinical manifestations, treatment, and follow-up. Gross features were recorded in each case from pathology reports and photographs of the gross specimens. Tumor stage was assessed according to the TNM system.
RESULTS
Clinical and pathologic findings(Table 1)
Clinical and pathologic data.
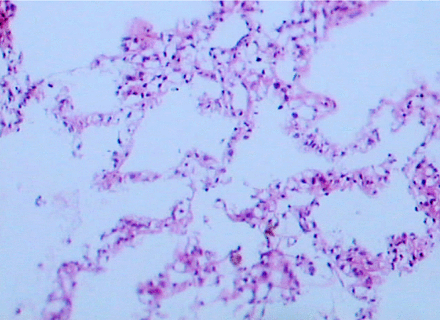
Of the 8 patients, there were 5 men (62.5%) and 3 women (37.5%). The mean age at diagnosis was 49.4 years. All cases were unilateral. The tumors were found incidentally during ultrasound evaluation for an unrelated condition in 5 patients (62.5%), for gross haematuria in one patient (12.5%), and for a renal cyst in the other 2 patients (25%) during follow-up. The overall mean greatest diameter of the MCRCC was 5.6 cm. Grossly, they consisted of a multiloculated lesion with a small thickened areas. The mean percentage of solid tumor component, estimated microscopically, was less than 25%. None showed any evidence of necrosis. The wall and septa were lined by one or several layers of clear cells in all cases with nuclear grade 1 in six (75%) and grade 2 in two cases (25%). All tumors were pT1, with the tumor limited in the kidney, no vascular involvement, no capsular penetration, no ipsilateral adrenal gland invasion, and no lymph node metastases.(Fig. 1) Four patients (50%) underwent radical nephrectomy, one (12.5%) partial nephrectomy, two(25%) laparoscopic nephrectomy, and one laparoscopic tumor enucleation.
Histologic examination revealed thin septa lined up by cuboidal clear cells (H&E×200).
Seven patients available for follow-up had survived tumor-free during the mean time of 8 months (range 6-18) with no evidence of metastasis or local spread.
Imaging studies
Renal ultrasound scans were available for all cases, and demonstrated a complex cystic mass in 7. A simple renal cyst was reported in one other patient. All 8 patients underwent IVU and renal CT scans, one had a normal IVU imaging, others showed distortion of the collecting system. CT showed a well-defined cystic mass with thin septa in 6 cases. Unenhanced CT scans revealed the cystic portions as hypodense in 6 tumors, but in the other two, hyperdense areas were admixed in some loculi. On enhanced CT scans, the solid portions in all except 3 were slightly enhanced, and the mean increase in CT attenuation in these cases was 20 Hu during the parenchyma phase. Cystic wall or septa calcification was found in 2 tumors.
DISCUSSION
At least 4–15% of renal tumors manifest primarily as a fluid-filled cystic mass on X-ray or ultrasonography. These tumors were generally named as “cystic renal cell carcinoma (CRCC)”, but the term of “CRCC” is actually unprecise because it refers to several lesions with differing histopathologic features and prognoses. Hartman et al. [2] classified CRCC into four types, of which, MCRCC was far different from unilocular cystic RCC and RCC with cystic degeneration in both prognosis and pathologic features. Thus, WHO recognized it as a distinct subtype of RCC in the 2004 classification. MCRCC has a reported incidence of 1-4% of the RCCs with a male predominance of 3:1 (62.5% of patients were males in the present series).
The pathologic criterion was modified in the 2004 WHO classification, and solid expansive nodules are no longer accepted for the diagnosis of MCRCC. The main pathologic features of MCRCC according to the 2004 WHO classification of kidney tumors were as follows: gross features including: multilocular cystic appearance and encapsulated; yellowish solid component limited to small areas; no expansive nodules; and no tumor necrosis present. Microscopic features including: cysts lined by cuboidal clear cells or flattened epithelium; septa containing aggregates of epithelial cells with clear cytoplasm; low Fuhrman grade. Furthermore, most pathologists agree that for the diagnosis of MCRCC, the neoplastic clear cells should occupy no more than 25% of the tumor volume.
Most MCRCC cases have no characteristic presentation. In our series, all except one who had he-maturia, were diagnosed incidentally during a health examination or the period of follow-up. Because the MCRCC is lacking in tumor components, fine-needle aspiration biopsy results in too many false negative results (reported 71%) for the lack of a sufficient number of good quality cores. In addition, there may be tumor spread along the needle track, cyst rupture, hemorrhage, and/or infection[3]. So it is not advisable to use this technique preoperatively for the diagnosis of MCRCC. While IVU and angiography may not be of much help for the diagnosis, ultrasonography and CT are the most practical tools for investigating and detecting MCRCC.
The sonographic appearance of MCRCC includes multiple anechoic spaces traversed by thin septa and no solid elements. Adding color Doppler may prove useful [4]. In our study, seven patients reported with a complex cystic renal mass, suggesting further evaluation. Combined with CT, ultrasound is a valuable tool for diagnosis and screening of MCRCC.
Based on CT findings, Isreal and Bosniak [5] classified cyst associated renal mass into five categories (Category I, II, II F, III, and IV). Category I are simple benign cysts and Category II are benign cystic lesions which are minimally complicated and need no intervention. Category I and V show some radiological features of malignancy, and should be explored surgically. Lesions of II F should be managed with follow-up. The Bosniak classification has been widely used to assist clinical decisions. In our study, seven tumors were Bosniak I and one was II F according to this classification. The CT imaging findings of our study and the literature are mainly described as follows:
Septa
Sebastien et al.[6] suggest that an expansile nodule of 5 mm or greater and irregularities of the tumor cyst wall and septa remain as the best imaging signs of CRCC. MCRCC, however, should be void of visible nodules, but with a number of regular thin wall and regular septa according to the WHO criteria. Two smaller lesions in our study, with so many septa within the tumors, become confluent and masslike. So CT is less reliable in evaluating MCRCC when the lesion is less than 4 cm in size, because it may appear as a solid mass. MR imaging is more sensitive than CT in demonstrating septa within a lesion.
Wall
Three tumors in our study had irregular wall thickening which is a relatively rare sign in MCRCC compared to other CRCCs. Such a sign may also be seen in nonneoplastic lesions, including an infected cyst, abscess, cyst with hemorrhage, pancreatic pseudocyst, and organizing hematoma with a pseudocapsule. Combined with the clinical presentation and other signs, differentiated diagnosis between MCRCC and these benign lesions is necessary.
Enhancement
The most important factor in the evaluation of a renal mass is the presence or absence of enhancement. A cystic renal mass is considered to be a neoplasm if there is an enhancing nodular septa within the lesion, especially when the change in attenuation is more than 15 HU after intravenous administration of contrast material.[7] Accurate measurement of the degree of enhancement in a thin wall and septa can be difficult because of the volume average effect. Thinner and overlapping sections have been suggested to decrease these artifacts.
Calcification
It has been demonstrated by Israel et al.[8] that calcification in a cystic renal mass is not as important in diagnosis as is the presence of associated enhancing soft-tissue elements. One showed thin-lined calcification in the wall and the other showed scattered calcification in the septa, which can not be distinguished from calcification presented in benign lesions.
Compared with necrotic CRCC and unilocular CRCC, MCRCCs contain fewer malignant cells, which seem to be proliferating at a slower rate. Furthermore, the majority of these tumors are grade 1 or 2 and has a low clinical stage (all pT1 in this study) at diagnosis, suggesting a tumor of low malignant potential. The prognosis of MCRCC is excellcent with a reported 5-year disease-related survival from 88.6% to 100% [9]. All seven patients available for followup in our study are alive tumor-free at present. Thus, patients with MCRCC might benefit from nephronsparing surgery. [10]
For tumors that cannot be determined preoperatively, if they are confused mainly with benign lesions, it may be appropriate to remove this lesion in a young patient (particularly if partial nephrectomy can be performed).This would alleviate patient anxiety and the need for long-term follow-up examinations. But in an elderly patient who is a poor surgical risk, a watchful waiting approach can sometimes be a prudent management choice. When it’s difficult to differentiate a multilocular cystic lesion from necrotic CRCC, a radical nephrectomy should be proposed for the reason that cystic degeneration of RCC predicts a poor prognosis and tumor progression. [11]
In summary, MCRCC should be recognized as a separate disease entity which appears to have a lower malignant potential and a better outcome. The benign clinical course of these lesions suggests that patients may benefit from nephron-sparing surgery, such as partial nephrectomy, either through open or laparoscopic surgery.
- Received November 27, 2006.
- Accepted February 2, 2007.
- Copyright © 2007 by Tianjin Medical University Cancer Institute & Hospital and Springer