Abstract
Purpose
The aim of this study is to investigate clinicopathologic characteristics and to identify prognostic factors in patients undergoing pulmonary metastasectomy for colorectal carcinoma.
Methods
This study is a single-institution retrospective study of 137 consecutive patients who underwent 158 pulmonary resections for metastatic colorectal carcinoma between January 1989 and June 2008.
Results
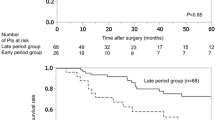
Median disease-free interval between colorectal resection and pulmonary metastasectomy was 35.6 months (range, 0.6 to 154.3 months). No perioperative deaths occurred. Follow-up was 100% complete and mean follow-up was 41.6 ± 27.6 months. Median survival was 36.2 months (range, 4.6 to 126 months). Overall 5- and 10-year survival rates were 55.4% and 30.8%, respectively, after pulmonary metastasectomy. At univariate analysis of patient survival, number of lung metastases (p = 0.002), disease-free interval of more than 24 month (p = 0.013), and absence of residual tumor (p = 0.024) were significant prognostic factors. At multivariate analysis, presence of solitary lung metastasis and disease-free interval of more than 24 months remained significant prognostic factors. There was no significant difference in the 5-year survival for 121 patients undergoing single thoracotomy compared with 16 patients undergoing repeated resection(s) for recurrent colorectal lung metastasis (55.1% vs 59.5%; p = 0.79). Nor was the presence of hepatic metastasis associated with lower outcome (p = 0.77).
Conclusions
Disease-free interval and number of metastases are the most significant prognostic factors for survival after pulmonary metastasectomy for colorectal carcinoma. Recurrent pulmonary disease can benefit from repeated resection. Prior hepatectomy for liver involvement does not influence survival.

Similar content being viewed by others
References
Ferlay J, Autier P, Boniol M, Heanue M, Colombet M, Boyle P (2007) Estimates of the cancer incidence and mortality in Europe in 2006. Ann Oncol 18:581–592. doi:10.1093/annonc/mdl498
Verdecchia A, Francisci S, Brenner H, Gatta G, Micheli A, Mangone L, EUROCARE-4 Working Group (2007) Recent cancer survival in Europe: a 2000-02 period analysis of EUROCARE-4 data. Lancet Oncol 8:784–796. doi:10.1016/S1470-2045(07)70246-2
Renehan AG, Egger M, Saunders MP, O'Dweyr ST (2002) Impact on survival of intensive follow up after curative resection for colorectal cancer: systematic review and meta-analysis of ramdomized trials. BMJ 324:813. doi:10.1136/bmj.324.7341.813
Manfredi S, Bouvier AM, Lepage C, Hatem C, Dancourt V, Faivre J (2006) Incidence and patterns of recurrence after resection for cure of colonic cancer in a well defined population. Brit J Surg 93:1115–1122. doi:10.1002/bjs.5349
Aberg T (1997) Selection mechanisms as major determinants of survival after pulmonary metastasectomy. Ann Thorac Surg 63:611–612. doi:10.1016/S0003-4975(97)00006-4
Treasure T (2008) Pulmonary metastasectomy for colorectal cancer: weak evidence and no randomized trial. Eur J Cardiothorac Surg 33:300–302. doi:10.1016/j.ejcts.2007.10.015
Pfannschmidt J, Dienemann H, Hoffmann H (2007) Surgical resection of pulmonary metastases from colorectal cancer: a systematic review of published series. Ann Thorac Surg 84:324–338. doi:10.1016/j.athoracsur.2007.02.093
Iizasa T, Suzuki M, Yoshida S, Motahashi S, Yasufuku K, Iyoda A, Shibuya K, Hiroshima K, Nakatani Y, Fujisawa T (2006) Prediction of prognosis and surgical indications for pulmonary metastasectomy from colorectal cancer. Ann Thorac Surg 82:254–260. doi:10.1016/j.athoracsur.2006.02.027
Onaitis MW, Petersen RP, Haney JC, Saltz L, Park B, Flores R, Rizk N, Bains MS, Dycoco J, D'Amico TA, Harpole DH, Kemeny N, Rusch VW, Downey R (2009) Prognostic factors for recurrence after pulmonary resection of colorectal cancer metastases. Ann Thorac Surg 87:1684–1689. doi:10.1016/j.athoracsur.2009.03.034
Melloni G, Doglioni C, Bandiera A, Carretta A, Ciriaco P, Arrigoni G, Zannini P (2006) Prognostic factors and analysis of microsatellite instability in resected pulmonary metastases from colorectal carcinoma. Ann Thorac Surg 81:2008–2013. doi:10.1016/j.athoracsur.2006.01.007
Inoue M, Ohta M, Iuchi K, Matsumura A, Ideguchi K, Yasumitsu T, Nakagawa K, Fukuhara K, Maeda H, Takeda S, Minami M, Ohno Y, Matsuda H (2004) Benefits of surgery for patients with pulmonary metastases from colorectal carcinoma. Ann Thorac Surg 78:238–244. doi:10.1016/j.athoracsur.2004.02.017
Pfannschmidt J, Muley T, Hoffmann H, Dienemann H (2003) Prognostic factors and survival after complete resection of pulmonary metastases from colorectal carcinoma: experiences in 167 patients. J Thorac Cardiovasc Surg 126:732–739. doi:10.1016/S0022-5223(03)00587-7
Kanemitsu Y, Kato T, Hirai T, Yasui K (2004) Preoperative probability model for predicting overall survival after resection of pulmonary metastases from colorectal cancer. Brit J Surg 91:112–120. doi:10.1002/bjs.4370
Yedibela S, Klein P, Feuchter K, Hoffmann M, Meyer T, Papadopoulos T, Göhl J, Hohenberger W (2006) Surgical management of pulmonary metastases from colorectal cancer in 153 patients. Ann Surg Oncol 13:1538–1544. doi:10.1245/s10434-006-9100-2
Zink S, Kayser G, Gabius H-J, Kayser K (2001) Survival, disease-free interval, and associated tumor features in patients with colon/rectal carcinomas and their resected intra-pulmonary metastases. Eur J Cardiothorac Surg 19:908–913. doi:10.1016/S1010-7940(01)00724-2
Saito Y, Omiya H, Kohno K, Kobayashi T, Itoi K, Teramachi M, Sasaki M, Suzuki H, Takao H, Nakade M (2002) Pulmonary metastasectomy for 165 patients with colorectal carcinoma: a prognostic assessment. J Thorac Cardiovasc Surg 124:1007–1013. doi:10.1067/mtc.2002.125165
Welter S, Jacobs J, Krbek T, Krebs B, Stamatis G (2007) Long-term survival after repeated resection of pulmonary metastases from colorectal cancer. Ann Thorac Surg 84:203–210. doi:10.1016/j.athoracsur.2007.03.028
Shah SA, Haddad R, Al-Sukhni W, Kim RD, Greig PD, Grant DR, Taylor BR, Langer B, Gallinger S, Wei AC (2006) Surgical resection of hepatic and pulmonary metastases from colorectal carcinoma. J Am Coll Surg 202:468–475. doi:10.1016/j.jamcollsurg.2005.11.008
Barlow AD, Nakas A, Pattenden C, Martin-Ucar AE, Dennison AR, Berry DP, Lloyd DM, Robertson GS, Waller DA (2009) Surgical treatment of combined hepatic and pulmonary colorectal cancer metastases. Eur J Surg Oncol 35:307–312. doi:10.1016/j.ejso.2008.06.012
Nakajima J, Murakawa T, Fukami T, Sano A, Sugiura M, Takamoto S (2007) Is finger palpation at operation indispensable for pulmonary metastasectomy in colorectal cancer? Ann Thorac Surg 84:1680–1684. doi:10.1016/j.athoracsur.2007.06.005
Nakas A, Klimatsidas MN, Entwisle J, Martin-Ucar AE, Waller DA (2009) Video-assisted versus open pulmonary metastasectomy: the surgeon's finger or the radiologist's eye? Eur J Cardiothorac Surg 36:469–474. doi:10.1016/j.ejcts.2009.03.050
Welter S, Jacobs J, Krbek T, Poettgen C, Stamatis G (2007) Prognostic impact of lymph node involvement in pulmonary metastases from colorectal cancer. Eur J Cardiothorac Surg 31:167–172. doi:10.1016/j.ejcts.2006.11.004
Rama N, Monteiro A, Bernardo JE, Eugénio L, Antunes MJ (2009) Lung metastases from colorectal cancer: surgical resection and prognostic factors. Eur J Cardiothorac Surg 35:444–449. doi:10.1016/j.ejcts.2008.10.047
Corman ML (2005) Carcinoma of the colon. In: Corman ML (ed) Colon and rectal surgery, 5th edn. Lippincott Williams & Wilkins, Philadelphia, p 871
Treasure T, Fallowfield L, Farewell V, Ferry D, Lees B, Leonard P, Macbeth F, Utley M (2009) Pulmonary metastasectomy in colorectal cancer: time for a trial. Eur J Surg Oncol 35:686–689. doi:10.1016/j.ejso.2008.12.005
Acknowledgements
We would like to thank Valentina Fava, (MSc) and Stefano Panetta, (MSc) for providing invaluable assistance in the statistical data analysis.
Conflict of Interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Borasio, P., Gisabella, M., Billé, A. et al. Role of surgical resection in colorectal lung metastases: analysis of 137 patients. Int J Colorectal Dis 26, 183–190 (2011). https://doi.org/10.1007/s00384-010-1075-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-010-1075-6