Abstract
OBJECTIVE To evaluate the clinical application of a right-thoracic approach with or without laparotomy for mid-upper esophageal cancer.
METHODS We retrospectively reviewed the data of 34 esophageal cancer patients who received Belsey surgery or a modified Ivor-Lewis surgery from November 1992 to April 2007. Twenty of the patients underwent a Belsey prodecdure (Group A) from November 1992 to January 2001 and 14 underwent a modified Ivor-Lewis prodecdure (Group B) from May 2001 to April 2007.
RESULTS Twenty patients with esophageal cancer received an esophagectomy through an exclusive right-thoracic approach (Belsey surgery), and 14 patients received an esophagectomy through a right-thoracic approach combined with a laparotomy (modified Ivor-Lewis surgery). The complication rate was 15% (3/20) and 7.1% (1/14) respectively. The survival rate was 42.9% (5-year survival) and 38.7% (5-year survival) respectively for these two groups.
CONCLUSION An exclusive right-thoracic approach (Belsey surgery) is associated with more complications. It is not a routine surgery for cancer of the mid-upper thorax of the esophagus, but can be selectively used as palliative esophagectomy for esophageal cancer patients with poor pulmonary function. Modified Ivor-Lewis surgery can simultaneously be utilized to resect the primary tumor and dissect lymph nodes of the thorax and abdomen. With a shorter time period of surgery and postoperative recovery period, modified Ivor-Lewis surgery can achieve better effects with patients who have midupper esophagus cancer.
keywords
Introduction
There are different surgical approaches for esophageal cancer worldwide. In Western countries, Ivor-Lewis and transhiatal esophagectomy (THE) are the primary methods[1]. Chen et al.[2] retrospectively studied 3,690 patients in China and found that 3,169 of the total received esophagectomy through a left-thoracic approach. Recently, there have been several articles about Belsey surgery and modified Ivor-Lewis surgery[3,4]. We retrospectively reviewed the data of 34 esophageal cancer patients who received a Belsey surgery or a modified Ivor-Lewis surgery from November 1992 to April 2007. The aim of this study was to evaluate the indication, morbidity and long-term outcomes of both types of surgeries.
Materials and methods
Clinical data
Thirty-four esophageal cancer patients received Belsey surgery or modified Ivor-Lewis surgery from November 1992 to April 2007. Twenty of this group underwent a Belsey prodecdure (Group A) from November 1992 to January 2001, and 14 underwent a modified Ivor-Lewis prodecdure (Group B) from May 2001 to April 2007. This study was approved by the surgical committee of the Cancer Hospital of Chinese Academy of Medical Sciences (Beijing, China).
There were 17 males and 3 females in group A with a median age of 58 (40~73 years). Seven patients had mid-thoracic esophageal cancer, and 13 patients had upper-thoracic esophageal cancer. According to UICC 2002 staging, 9 patients had a pathological Stage II disease and 11 patients were at Stage III.
In group B, there were 12 males and 2 females with a median age of 66 (58~78 years). Five patients had mid-thoracic esophageal cancer, and 9 patients had upper-thoracic esophageal cancer. The pathological stages were as follows: 1 patient, Stage I; 2 patients, Stage II; and 11 patients Stage III. The histological type was squamous cell carcinoma in all of the patients.
Surgery
Group A
Esophagectomy through an exclusive right-thoracic approach (Belsey surgery, 1974). In brief, after the esophageal lesion was resected, the stomach was mobilized through the hiatus and pulled up into the chest. An anastomosis was established between the esophageal remnant and the stomach in the right thorax.
Group B
Modified Ivor-Lewis surgery. A classic Ivor-Lewis surgery, after stomach mobilization was performed through a laparotomy. The patient was placed in the left decubitus position and right thoracotomy was performed. After the stomach was pulled up into the chest, an anastomosis was established between the esophagus and the stomach in the right thorax. We modified the classic Ivor-Lewis surgery as follows: the right thoracotomy was conducted first. If it was definitive that the lesion would be dissected after exploration, the operation bed was titled to the chief surgeon and a median laparotomy was performed. After the stomach was pulled up into the chest, an anastomosis was established between the esophagus and the stomach in the right thorax using a stapling device.
Statistical analysis
The survival was calculated by the Kaplan-Meier method using SPSS 13.0 software.
Results
Morbidity and mortality
The overall morbidity rate was 15% (3/20) in group A, in which 2 patients had an anastomotic leak, and 1 patient had bleeding in the abdomen. One patient died of a myocardical infarction on the 4th day after operation. The overall morbidity rate was 7.1% (1/14) in group B, in which 1 patient suffered from a postoperative stress ulcer. No deaths occurred postoperatively.
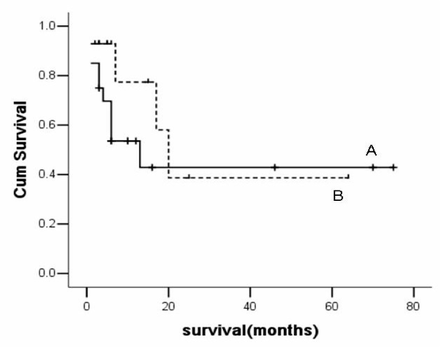
The median survival was 10 months (3~75 months) in group A, and 5-year survival was 42.9% (Fig.1). The median survival was 11 months (3~36 months) in group B, and 5-year survival was 38.7% (Fig.1).
Acturial 5-year survival was 42.9% for patients receiving Belsey surgery (A) and 38.7% for patients receiving modified Ivor-Lewis surgery (B).
Discussion
There are many surgical approaches for esophageal cancer. Two types of route may be used: a transthoracic (right or left) or a transhiatal route. Recently, minially invasive esophagectomy (MIE)[5] was reported to be safe and comparable to an open approach with respect to postoperative recovery and cancer survival, but the sample number was relatively small. Ivor-Lewis surgery and transhiatal[6] esophagectomy are two main surgeries in Western countries, whereas esophagectomy through a left-sided approach is the predominant approach in China, as noted by Chen et al.[2], who reported that 87.3% (3,169/3,630) patients received esophagectomies through a left-sided approach.
With regard to the choice of surgical approaches, it is based on the site of the lesion, general condition of the patients and the proference of the surgeons[1]. Though there are advantages and disadvantages between a varity of surgical procedures, two principles regarding resection should be noted: R0 resection(removal of all macroscopic and microscopic tumor) and resection of lymph nodes. Yekebas et al.[7] recently showed that compared to transhiatal esophagectomy, transthoracic radical en-bloc esophagectomy can increase 5-year survival of esophageal cancer patients if there are no micro-metastases. They also showed the necessity of radical resecton of the primaty tumor and lymph nodes.
Belsey surgery was first reported in 1974. He had operated on 140 cases of esophageal cancer using an exclusive right thoracic approach. Since then, no furthur reports appeared in Western countries, but rare reports were found in China[8,9]. The morbidity rate was reported to be 0~28.1%, the most common complications being anastomotic leakage, pulmonary infectons and delayed intrathoracic stomach emptying. The morbidity rate in our study was within the range of that reported in the literature, and 5-year survival was also similar to survival from a large series of esophagectomies for esophageal cancer[2]. Belsey surgery has the advantage of a more efficient approach with minimal injury, shortened operation time and less pain[4,8]. But it is difficult to resect abdominal lymph nodes, especially the left gastric lymph nodes by this prodecure, so it is not in accord with surgical oncological principles. Based on the literature and our data, we conclud that Belsey surgery is not a preferred procedure for mid-thoracic esophageal cancer, but it can be selectively used as a palliative procedure for mid-thoracic esophageal cancer.
Owing to dissecting a primary lesion and the lymph nodes of the thoracic and abdominal fields, Ivor-Lewis surgery has been a “standard operation” for esophageal cancer in Western countries since 1946. Recently, there have been increasing reports regarding esophagectomy for esophageal cancer using Ivor-Lewis surgery in China[3,10-12]. The morbidity rate has been reported to be 7.3~16%, and 5-year survival rate between 30~48.8%. It has the advantage of a complete resection of the esophageal cancer and recurrent nerve lymph nodes, and post-aortic and supra-aortic lymph nodes which can not be approached through a left-sided thoracic incision[12]. In order to overcome the disadvantage of changing the patients’ position intraoperatively, we modified the procedure as follows: right thoracotomy was performed first, then if it was definitive that the lesion would be dissected after exploration, the operation bed was titled to the chief surgeon and a laparotomy was conducted, After the stomach was pulled up into the chest, an anastomosis is connected between the esophagus and stomach in the right thorax using a stapling device. We named it as a modified Ivor-Lewis surgery. It has several advantages over classic Ivor-Lewis surgery. First, if the esophageal lesion can not be resected, then surgery would terminate, avoiding injury from laparotomy. Second, a modified Ivor-Lewis surgery shortened the operation time which benefits patients’ recovery. In spite of the low morbidity rate, our limited data need further investigation due to a relative short follow-up period.
Similar to classic Ivor-Lewis surgery, modified Ivor-Lewis surgery may also be employed to resect a primary tumor and lymph nodes simutaneously from the mediastinal and abdominal fields, and it is especially appopriate for mid-upper thoracic esophageal cancer. The differences between our modified Ivor-Lewis surgery and the modified Ivor-Lewis surgery of Wang et al.[3] and Lu et al.[9] lie in that in the latter operation, they commence the thoracotomy and laparotomy simutaneously, whereas we do not conduct palliative esophagectomy if the esophageal lesion cannot be resected completely. We recommend a non-operative treatment such as radiotherapy and stent for these patients.
- Received November 20, 2007.
- Accepted January 10, 2008.
- Copyright © 2008 by Tianjin Medical University Cancer Institute & Hospital and Springer